As the saying goes, “We gain three pounds during the festive season”, and the National Day is coming soon. I think everyone will start shopping or eating while lying down.
To lose weight, it is necessary not only to “stretch your legs”, but also to “keep your mouth shut”, but it is easy to say in words, but difficult to do in practice…
p>It is even more unfortunate that for us “clockers”, how to control diet reasonably has always been a super problem compared to physical exercise.
But sometimes, obesity is not just because we can’t eat, it can also be affected by metabolic syndrome [1]. Metabolic syndrome refers to the pathological state of metabolic disorder of proteins, fats, carbohydrates and other substances in the human body. And Dietary restriction(DR)is an effective means to help patients with metabolic syndrome lose weight and self-renewal.
However, there is still a lack of understanding of how dietary restriction “cures” metabolic syndrome: is it the burning of calories that leads to an improvement in metabolism? Or did changes in nutrient intake reconstruct a new look of metabolism [2-3]?
A study published online in Nutrients on June 28, 2022 by Maria Cristina Foss-Freitas’ team at the University of São Paulo (USP) in Brazil, reveals the contribution of dietary restriction to the treatment of metabolic syndrome. Effective approach: protein restriction (PR) can improve metabolic syndrome, reduce body weight, blood sugar, blood lipids, blood pressure, and effectively improve insulin sensitivity, similar to calorie restriction (CR) positive feedback. Meanwhile, the PR pathway did not appear to cause redundant body damage, the population diversity of fecal microbes was unaffected by the intervention, and adipose tissue transcriptome changes were weak.

In order to obtain first-hand available material to analyze the contribution of PR (protein intake restriction) and CR (calorie restriction) regimens to metabolic syndrome, researchers recruited 150 patients with metabolic syndrome , after excluding biased individuals and considering personal wishes, 40 patients were included in the total number of initial patients, and the following experimental scheme was formulated: the calorie intake in the CR group was reduced by 25%, and the balance of dietary structure remained unchanged; the calorie intake in the PR group remained unchanged, but Dietary changes, protein intake reduced by 50%. After 27 days of experimentation, 11 participants completed the CR protocol and 10 completed the PR protocol.
First, the researchers looked at changes in body weight, anthropometric and energy-related parameters before and after the experiment. Both CR and PR groups showed a reduction in body weight, fat mass, waist and hip circumference, but not muscle mass (Figure 1). The CR group showed slightly more prominent performance in energy consumption, the ability to consume energy was stronger, and the changes in VO2 (oxygen uptake), VCO2 (carbon dioxide) were also more significant (Figure 1).
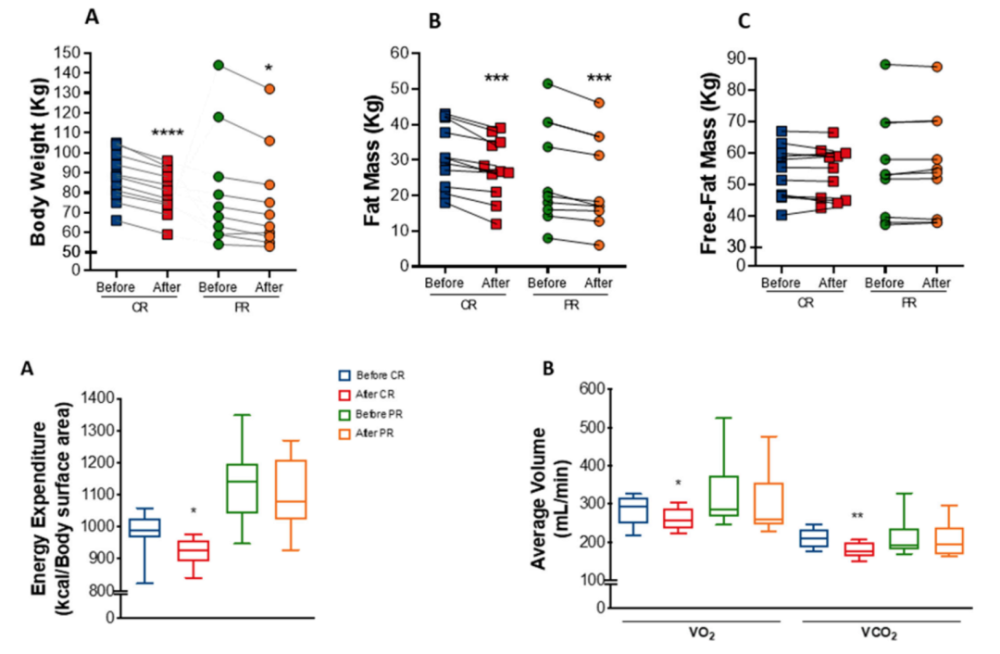
Figure 1: Changes in body weight, anthropometrics, energy, etc. of participants after CR and PR regimens
Importantly, the investigators found that both PR and CR regimens reduced blood pressure and heart rate in patients with metabolic syndrome and reduced the risk of cardiovascular disease (Figure 2).
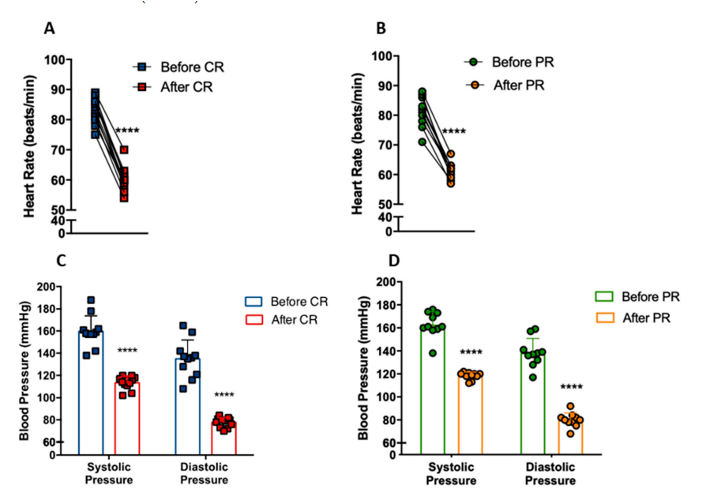
Figure 2: Changes in participants’ heart rate and blood pressure after CR and PR regimens
In terms of biochemical parameters, after the CR and PR regimens, the fasting blood glucose of the patients was reduced by more than half, the hemoglobin was only slightly reduced, and the total hemoglobin and hematocrit levels did not change. Significantly. In the cholesterol analysis, total cholesterol, low-density lipoprotein cholesterol decreased. The realization of inflammation in the CR and PR regimens is also worthy of attention, greatly alleviating people’s concerns about “dieting affects health”. Inflammatory markers and muscle damage markers decreased in the two groups, while liver damage markers did not change significantly.
In addition, PR and CR procedures significantly improved insulin sensitivity in patients with metabolic syndrome, i.e. increased glucose infusion rates (Figure 3). The homeostatic model of β-cell function (HOMA-beta) was increased and the homeostatic model of insulin resistance (HOMA-ir) was decreased under the CR versus PR protocol.
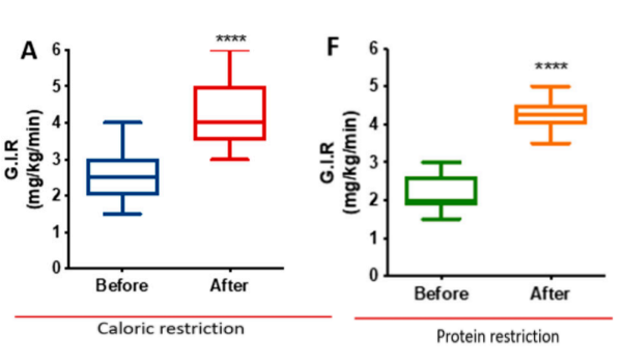
Figure 3: Participants’ performance after CR and PRIncreased insulin sensitivity
In the above-mentioned parametric test, the PR protocol has a promising performance as a novel dietary control protocol, and the changes in these symptoms are not temporary, and can last at least until the end of the patient one month after the agreement. Moreover, the analysis of fecal samples after the PR program showed that there was no significant change in the microbial diversity. Further, the researchers performed bulk transcriptome analysis on the adipose tissue of CR and PR participants, and the results showed that there was no significant change in the adipose transcriptome.
Which factors drive metabolic improvements in dietary restriction? This article brings us a new answer: restricting protein intake can simulate calorie intake in many ways and help patients with metabolic syndrome to control health parameters such as weight, blood sugar, blood lipids, and blood pressure. Considering the simplicity of PR operation, this may be a more effective, easier and more promising metabolic adjustment protocol, which has become a boon for patients with metabolic syndrome (Figure 4).
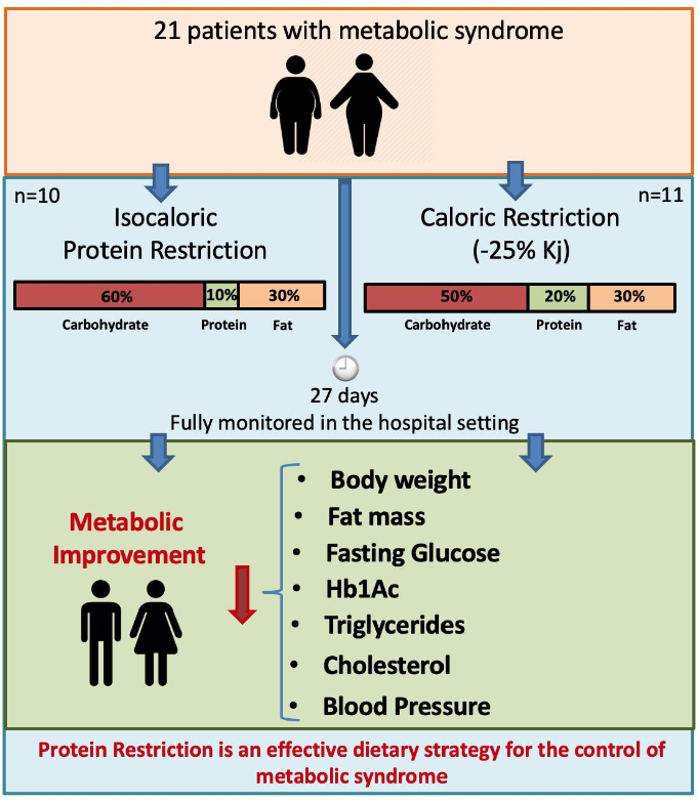
Figure 4: The PR scheme can highly mimic the CR scheme in many ways
This study has brought us a piece of good news, in the case of “keep your mouth shut”, properly adjusting the diet structure and reducing protein intake can still control your weight and keep your body healthy ! But the researchers stressed that this study is only applicable to people with metabolic syndrome, and it is uncertain whether it will be applicable to everyone.
References:
1.Mooradian, A.D. Dyslipidemia in type 2 diabetes mellitus. Nat. Clin. Pract. Endocrinol. Metab. 2009, 5, 150–159.
2. Anderson, R.M.; Weindruch, R. Metabolic reprogramming in dietary restriction. Interdiscip. Top. Gerontol. 2007, 35, 18–38
3. Newgard, C.B.; An, J.; Bain, J.R.; Muehlbauer, M.J.; Stevens, R.D.; Lien, L.F.; Haqq, A.M.; Shah, S.H.; Arlotto, M.; Slentz, C.A.; et al. A branched-chain amino acid-related metabolic signature that differentiates obese and lean humans and contributes to insulin resistance. Cell Metab. 2009, 9, 311–326.
Writing|A Potato
Editing|Little Ears