A netizen consulted online: I had a chest CT during the recent physical examination, and the report said 7mm solid pulmonary nodule, RADS grade 3, I don’t know what this grade 3 means? Will it be malignant?
I believe that many patients who have found nodules want to know whether their nodules are malignant or not, but sometimes it is difficult to find a doctor, and they have to queue up at the hospital to register, thinking about the crowds in the hospital. The scene is prohibitive, and I find it unreliable to look for popular science on the Internet to compare, and the popular science articles are mixed. If you try to get rid of the traps mentioned in the article and feel that there is nothing to be trapped, what should you do at this time? Take a look at the RADS grading on the CT report.
RADS grading of pulmonary nodules is a way of classifying pulmonary nodules. It is usually based on the size, density, morphological status and growth rate of the nodules under CT. for 6 levels. Its purpose is to assist in the assessment of benign and malignant pulmonary nodules, or to determine whether high-risk or low-risk nodules.
Class 1 (negative, probability of malignancy
No pulmonary nodules or pulmonary nodules determined to be benign (with benign calcifications or fat). Such nodules are considered low-risk and require only 12 months of annual low-dose chest CT follow-up.
Class 2 (benign nodules, malignant probability <1%)
Mostly benign nodules with a low probability of developing into clinically aggressive lung cancer usually include 8 conditions, namely benign calcified nodules, interlobar fissure nodules, lipid-containing nodules Hamartomas, spherical atelectasis, nodules benign on biopsy, nodules within 5 mm, subsolid density nodules ≥5 mm in diameter with stable follow-up for more than 5 years or solid density nodules ≥5 mm stable with follow-up More than 2 years, it is also a type 2 pulmonary nodules, and this type of pulmonary nodules can also be reviewed regularly for 12 months.
Class 3 (uncharacterized nodules, 1-2% probability of malignancy)
For newly or initially screened nodules larger than 10 mm in diameter, CT examination may appear blurred or ground-glass edges, partial ground-glass density, tree-in-bud sign, satellite lesions and other features. classified into three types of nodules. A stable solid nodule within 2 years of follow-up or a stable subsolid nodule with a follow-up period of less than 5 years was also classified as a category 3 pulmonary nodule if the nodule diameter was between 5 and 9 mm. Treatment: 6-month follow-up review is generally recommended.
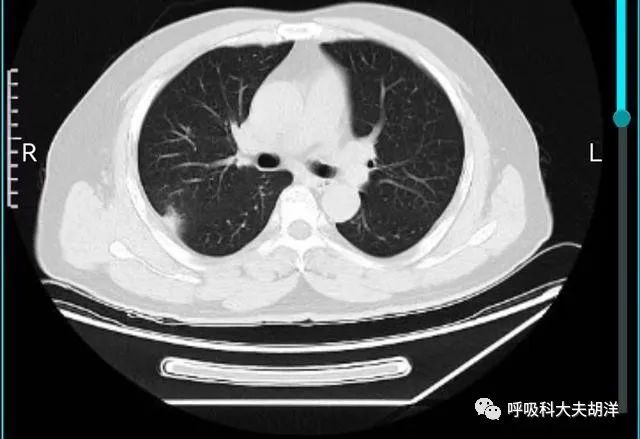
Class 4 (suspected malignant nodules)
Class 4 nodules are further subdivided into three types: 4a, 4b, and 4c. Class 4a nodules are 10-25 mm solid nodules with unclear benign features. The probability of malignancy is 5-15%. Management: 3-month low-dose chest CT screening; PET/CT examination if there is a solid component ≥8 mm.
Class 4b nodules are persistent subsolid density nodules ≥10 mm in diameter with a solid component ≤5 mm. The probability of malignancy is >15%. It may be carcinoma in situ or minimally invasive carcinoma. Management: Enhanced chest CT or plain target scan; selective PET/CT and/or tissue biopsy according to the probability of malignancy and complications; PET/CT if there is a solid component ≥8 mm.
4c has a higher rate of malignancy and is usually a partially solid nodule (solid component ≥5 mm) that does not improve significantly at short-term follow-up. Nodules ≥10 mm in diameter with clear borders, lobulations and spurs, and no inflammatory lesions were also defined as category 4C pulmonary nodules. The treatment is the same as for category 4b.
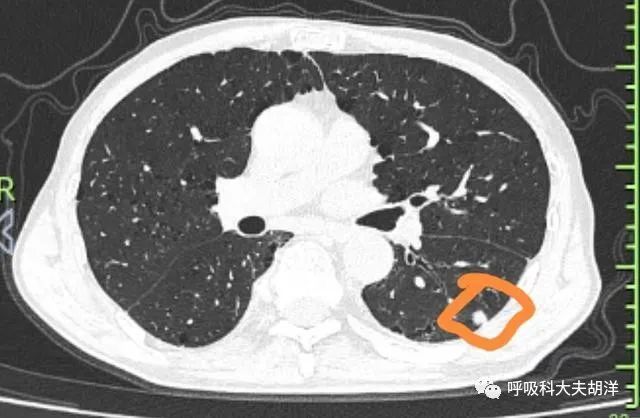
5 classes
Type 5 pulmonary nodules are those that are strongly suggested to be malignant nodules during CT examination. It is recommended to perform pathological examination or surgery as soon as possible, and selectively perform PET-CT.
Class 6
Type 6 pulmonary nodules are defined as malignant nodules by histological examinations such as fine needle aspiration cytology and central biopsy. Early surgery is recommended, and PET-CT can be optionally performed.
The classification of nodules is actually dynamic. For example, nodules that were classified as Class 2 at the initial screening, if they increase during follow-up and the solid component increases, they may be classified into Class 4 later. For the judgment of benign and malignant pulmonary nodules, the more important thing is to follow up and compare before and after. In addition, comprehensive judgment should be made based on whether there is a family history of lung cancer, whether there is long-term smoking, occupational exposure and other high-risk factors for lung cancer.