
While the COVID-19 fatality rate has grabbed most of the attention over the past two years, another epidemic is also continuing to mercilessly approach the United States—people are being driven by excesses Died from taking opioids. A total of 68,630 opioid overdose deaths were recorded in 2020, caused in part by forced quarantines and social distancing; higher than in 2020.
But the COVID-19 pandemic may have a seemingly paradoxical benefit for opioid-addicted people: offline healthcare is no longer safe because of the pandemic, so telehealth in the U.S. has eased Regulation has made many services, including addiction treatment, an online option. As a result, people with opioid use disorder receive more nationwide drug treatment and support than ever before. While it’s too early to know if this is more beneficial for people to wean themselves off drugs, early signs are showing promising results.
The federal government estimates that 2.7 million Americans have opioid use disorder (i.e., opioid addiction), which is nearly 1 percent of the population. It is a chronic brain disease caused by repeated use of prescription opioids such as hydrocodone, oxycodone, morphine or illicit drugs such as fentanyl and heroin formed. People with opioid use disorder are 20 times more likely to die from a drug overdose, infectious disease, trauma or suicide.
– Thierry Fousse-
Fortunately, methadone and buprenorphine, two FDA-approved drugs, can help patients improve withdrawal symptoms and control or eliminate compulsions Opioid use. Eric Weintraub, chief of the Division of Alcohol and Drugs at the University of Maryland School of Medicine, noted that patients who received these drugs fared better in many ways than those who did not. They had fewer overdoses and injections, a lower risk of disease transmission, less criminal activity, lower rates of illicit drug use, and higher rates of treatment maintenance. Indeed, people with opioid use disorder who received long-term methadone or buprenorphine treatment had a 50 percent drop in the rate of death from drug overdose.
Oregon Health and Science University addiction researcher Dennis McCarty co-authored a 2018 Annual Review of Public Health A review of opioid use disorder treatment*, he said, “The first thing you have to do is give the patient access to medication, and then you can go to them to discuss needs such as psychotherapy—but First, please get them medicine.”
*Translator’s Note
McCarty, Dennis, Kelsey C. Priest, and P. Todd Korthuis. “Treatment and prevention of opioid use disorder: challenges and opportunities.” Annual Review of Public Health39 (2018): 525.
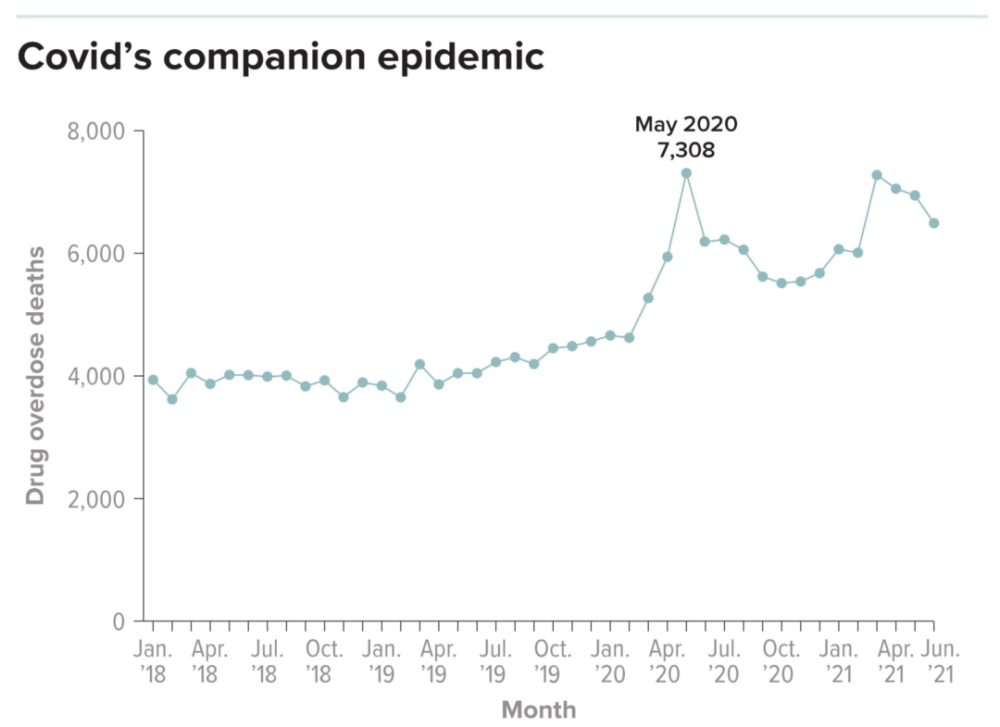
The opioid death rate in the U.S. has hit a new high during the COVID-19 pandemic, driven in part by isolation and social distancing.
—
J.C. Baumgartner & D.C. Radley / COMMONWEALTH FUND 2022 Knowable Magazine
According to the National Survey on Drug Use and Health, only 19 percent of adults with opioid use disorder were receiving medication in 2019. A big reason for this is that regulations require doctors to meet with patients before prescribing drugs. As a result, many people, especially those living in rural areas, have difficulty accessing treatment. For example, nearly 90 percent of rural communities have few eligible treatment programs, and about 30 percent of Americans live in counties without buprenorphine providers.
Baltimore-based Weintraib and his colleagues traveled 70 miles to Denton, Maryland, to visit patients with opioid use disorder at the Caroline County Health Department. “We’ve found people who live in Fort Friders and Greensboro, which are only 15 to 20 minutes away, but can’t come here for treatment because of the lack of public transportation,” Weintraeb said. Even drive a tractor or bike to therapy.
Barriers to buprenorphine treatment in early 2020 COVID-19Love began to break down when it first swept the United States. Shortly after the government declared the COVID-19 outbreak an official public health emergency, it eased controls on buprenorphine, allowing licensed doctors to prescribe telemedicine without first seeing patients in person Get a prescription for buprenorphine. This is also the first time that telehealth services have been available across state lines, giving patients access to physicians across the country. Government and private insurers have also agreed to pay for telehealth services. These changes have prompted drug providers to rapidly turn to telehealth, helping residents of their communities receive care in new ways.

Telehealth offers people the opportunity to receive treatment for opioid use disorder remotely, privately, and often without the knowledge of family members and neighbors. Some small studies have shown that online treatments are as effective as traditional offline treatments, although experts stress that more research is needed.
—
pixabay
At Sadler Health Center in South Central Pennsylvania, for example, prior to the outbreak, patients seeking treatment had to submit urine samples for drug screening before each appointment . All sessions are face-to-face and last from a week to a month, depending on the stage of the patient’s recovery. When the pandemic hit, Pennsylvania no longer required drug screening, and the federal government allowed Seidler’s clinicians to prescribe drugs through telehealth without an initial visit.
The pre-pandemic for-profit companies that saw opportunity in the huge but unmet needs of people with opioid disorders, today, in addition to traditional suppliers such as Seidler , they also began to expand rapidly. McCarty argues that the rule change, which has allowed companies to prescribe remotely, has allowed them to explode.
As of early 2020, for example, Bicycle Health, founded in 2017 in Redwood City, California, has only one clinic serving a dozen or so nearby residents. Previously, treatment and support services were provided online after a patient first saw a doctor and received a prescription. However, when in-person visits were no longer necessary during the pandemic, Bicycle Health has grown and now serves more than 10,000 patients in 23 states. Companies including Halcyon Health, Bright Heart Health, Ophelia, Workit Health and Eleanor Health also serve patients in multiple states via phone software or webcams.
Although online therapy removes barriers to initiating drug treatment for some opioid addicts, researchers aren’t sure if it’s as effective as in-person therapy in ongoing therapy. McCarty and colleagues recently reviewed nine studies to determine the effectiveness of telemedicine in medication-assisted treatment* for opioid use disorder. In every study they looked at, telehealth programs were as effective as offline treatment in adhering to medication and treatment maintenance, as well as reducing rates of illicit drug use.
*Translator’s Note
Medication-Assisted Treatment (MAT), a combination of medication, counseling, and behavioral therapy, has been shown to be clinically effective in the treatment of opioid use disorder.
However, they point out, none of these studies are very robust, as few clinicians were using teletherapy before the pandemic. The researchers found only two randomised controlled trials from those studies (which are often seen as the strongest study designs), and both had very few participants; Observational description of one of the programs (remote or offline therapy), which also mostly had few participants.

Many small towns lack opioid addiction treatment programs. This limits the opportunities for people living outside the big cities to seek help. Denton, Maryland, had treatment programs before the pandemic, but even residents of nearby towns struggled to get there. For rural residents, online therapy programs are very beneficial.
—
USDA Photo by PRESTON KERES / FLICKR
Studies comparing offline treatment of opioid addiction before the pandemic with teletherapy during the pandemic are emerging. At a rural health center in Pennsylvania that switched to teletherapy, 91 percent of patients were still on the program after three months, compared with 94 percent of the in-person program before the pandemic. More solid evidence is coming, thanks to a large-scale study of virtual treatment for opioid use disorder launched by the National Substance Abuse Treatment Clinical Trials Network. We will see results in a few years.
Bright Heart Health’s chief medical officer, David Kan, believes that research on telemedicine in general has encouraged the use of opioid use disorders. “Research around telemedicine, regardless of the disease, has shown that people can do as well in telemedicine as they do in-person, and consumer satisfaction has even improved,” he said. Ken also mentioned A review article* that reviewed 13 studies examining psychotherapy and medication prescriptions delivered through telehealth to address nicotine, alcohol, and opioid use disorders. The review authors concluded that most patients are satisfied with teletherapy and, therefore, teletherapy is a very effective alternative—especially in situations where in-person therapy may not be practical.
*Translator’s Note
Lin, Lewei Allison, et al. “Telemedicine-delivered treatment interventions for substance use disorders: A systematic review.”Journal of substance abuse treatment101 (2019): 38-49.
Ken points out: “With regard to the treatment of opioid use disorder, it is clear that patients prefer online treatment. We must make it easier to access treatment than to obtain addictive drugs. Otherwise, continued use of addictive drugs becomes a more attractive option.”

– Somewan-
Although medication is the best evidence-based therapy, says Shannon Schwoeble, manager of the
Bicycle Health rehabilitation coaching program )*, but most patients still require psychotherapy and other support. She oversees 24 peer-led online support groups where patients can seek help six days a week. She believes that online treatment has more benefits than offline treatment. “Most of their stories were like, ‘I’m embarrassed and I don’t want people to see me walking into the clinic’ or ‘I’m not going to let my family know I’m doing something like this, but I really need to It, because I know it will help me.'”
*Translator’s Note
Evidence-based therapy should be clinical based on the strongest available scientific evidence (eg, clinical research evidence is superior to basic theory or animal test evidence). practice, not medical decisions based on the physician’s personal experience, etc.
Schwebel, who is in long-term recovery himself, says prescription drugs can reduce cravings, “after which the real work begins, and you can start to gradually move away from the Your use of (addictive) drugs.”
Patients might wonder if they would receive effective support through the Zoom platform alone, but Schwebel sees it as useful. “You have a computer and you can temporarily detach yourself,” she said. “With us, you can see people from all parts of the country, from all groups, from all walks of life coming together and helping each other.”

– Tamuna Gogoladze –
New York-based Foundation for Opioid Response Efforts (FORE) provides grants to organizations battling the opioid epidemic in the U.S. FORE Physician and Director According to Karen Scott, remote healing may not work for everyone. FORE focuses on programs targeting the highest-risk opioid users because most of these users have other social or mental health issues and other issues that must be addressed along with their addictive behaviors.
Scott said, “In this case, a 15-minute visit and a prescription for buprenorphine are not enough. For those at risk of death and risk of forgoing treatment For very tall people, they need a whole package of wraparound services and a relationship building.”
Some organizations receiving FORE grants did use teletherapy to contact patients early in the pandemic. “But based on what we’ve heard from the subsidized organizations, they’re very anxious to get back to in-person visits early and safely because they’re very concerned,” Scott said.
Today, the relaxation of teletherapy regulations can only last until the end of the government-declared public health emergency. McCarty and other experts expect the rules allowing telehealth, at least for opioid use disorder, to persist. But that prediction has yet to come to fruition, putting the current surge in online treatment programs at risk.
Considering that approximately 2 million Americans require treatment services, 90% of whom do not receive treatment,Bicycle Health Ankit Gupta, founder of , said: “I don’t know how else I could fill this void without teletherapy.”
Author: Lola Butcher l Translator: Muchunl Proofreader: M. W.
Editor: egggriell Typesetting: Wen Ying l Cover: Katrin Emery
Original:
https:https://knowablemagazine.org/article/mind/2022/does-online-opioid-treatment-work


