Breast cancer is the most common malignancy in women, and after diagnosis, molecular testing is performed to determine the type of breast cancer. According to genetic characteristics and current treatment methods, it can be divided into three categories: hormone receptor-positive, HER2-positive and triple-negative breast cancer. These three types of cancer have many differences in how they are treated and how long patients live.
Testing for HER2 in breast cancer
HER2, also known as epidermal growth factor receptor-2, HER2-positive breast cancer, as the name suggests, refers to the overexpression of human epidermal growth factor receptor HER2 in the tumor, or the presence of amplification of the HER2 gene . Cancer cells grow rapidly and metastasize more easily. This type of breast cancer accounts for about 15%-20%.
The detection of HER2 is generally analyzed by immunohistochemistry. If it is three plus signs, it is judged to be HER2 positive. If HER2 is two plus signs, it needs to be in situ Immunofluorescence hybridization was used to verify whether it was HER2-positive breast cancer.
If the HER2 detected by immunohistochemistry shows a plus sign, it is generally considered to be HER2 negative, and these patients are not recommended to use HER2-targeting therapeutic drugs, such as trastuzumab, paclitaxel Tocilizumab, etc.
However, some researchers believe that due to the heterogeneity of tumors, the detection results of HER2 may be affected by sampling, so even if one or two plus signs of HER2 are detected, it cannot be simply These patients are still likely to benefit from targeted therapy.
Learn about the detection and expression of HER2. The anticancer drug DS-8201a to be introduced next is a new type of monoclonal antibody conjugated drug targeting HER2. It is reported that DS-8201a has a certain curative effect in the treatment of breast cancer with low expression of HER2. The following cancer degree will share a case to let everyone know the magic of DS-8201a.
A 23-year-old patient’s difficult journey against cancer
In January 2014, a 23-year-old woman presented with a 10-centimeter mass in the right breast, which was diagnosed as invasive ductal carcinoma on biopsy. Molecular testing was found to be ER (estrogen receptor) positive, PR (progesterone receptor) negative, and immunohistochemistry for HER2 was two plus signs, but was negative by in situ immunofluorescence hybridization (FISH). Genetic testing found negative for the BRCA1, BRCA2 and TP53 genes, and the patient did not have the cancer for a known genetic cause.
Bone scan revealed that the patient had thoracic vertebral metastases, and 4 cycles of chemotherapy with epirubicin and cyclophosphamide were started for this purpose. This was followed by treatment with goserelin and paclitaxel. A right breast tumor resection was performed, and axillary lymph nodes were dissected. The patient achieved progression-free survival of 17 months after surgery with radiotherapy and endocrine therapy.
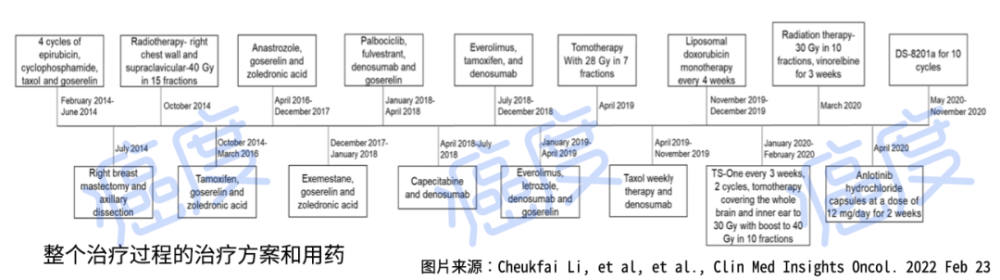 Figure 1. Treatment plan and medication throughout the course of treatment
Figure 1. Treatment plan and medication throughout the course of treatment
However, the disease did not let go of the young patient easily, and the disease progressed with bone metastases. For this reason, patients were started using CDK4/6 inhibitors, endocrine therapy, targeted therapy, chemotherapy-grade radiotherapy, etc. Despite the continuous attempts of various treatments, the condition continued to progress.
In November 2019, metastases were found in the patient’s liver, lymph nodes, and nasopharynx. In January 2020, the patient lost hearing in the left ear and subsequently developed nausea and dizziness. With abnormally elevated tumor markers and multiple brain metastases detected by contrast-enhanced MRI, she began chemotherapy and radiation therapy.
A biopsy of metastases in the liver revealed triple-negative breast cancer, which was different from the 2014 diagnosis of the disease. In February 2020, liver samples were re-sampled and tested, and the results were negative for ER, 10% positive for PR, a plus for HER2, and highly heterogeneous.
In March 2020, patients began treatment with the anti-angiogenic targeted drug anlotinib as tumor markers began to soar.
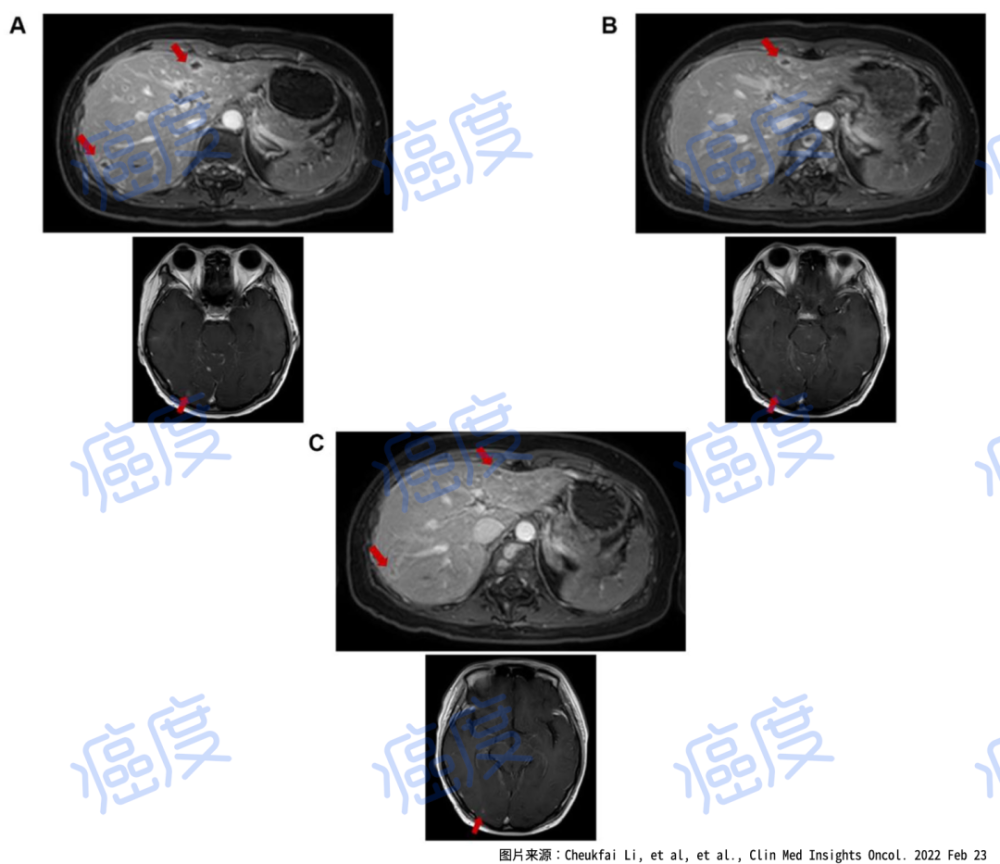 Figure 2. MRI results of brain and liver
Figure 2. MRI results of brain and liver
On May 4, 2020, tumor markers continued to rise and liver function was abnormal. After discussion with clinicians, DS-8201a was administered to the patient. After one cycle of medication, the pain disappeared and the patient was able to get up and walk. Later, several courses of DS-8201a were continued. After the sixth treatment cycle, the MRI of the brain showed that the lesions shrunk, the metastases in other parts of the body were significantly reduced, and the tumor markers also decreased rapidly.
On September 28, 2020, brain MRI showed that the meningeal metastases were progressing, but the parenchymal metastases were shrinking. Whole brain radiation therapy was no longer suitable because the patient had previously undergone whole brain radiation therapy. For this reason, DS-8201a can only be continued, with endocrine and symptomatic treatment at the same time.
On November 19, 2020, the patient stopped using DS-8201a for ten cycles and began to switch to palliative care. The patient unfortunately passed away in April 2021.
When the patient’s condition continued to progress, there were multiple metastases throughout the body, and even meningeal metastases had occurred, and there was almost no cure, the use of DS-8201a extended the patient’s 11 month lifetime. The final result made us regret, but also gave us some inspiration.
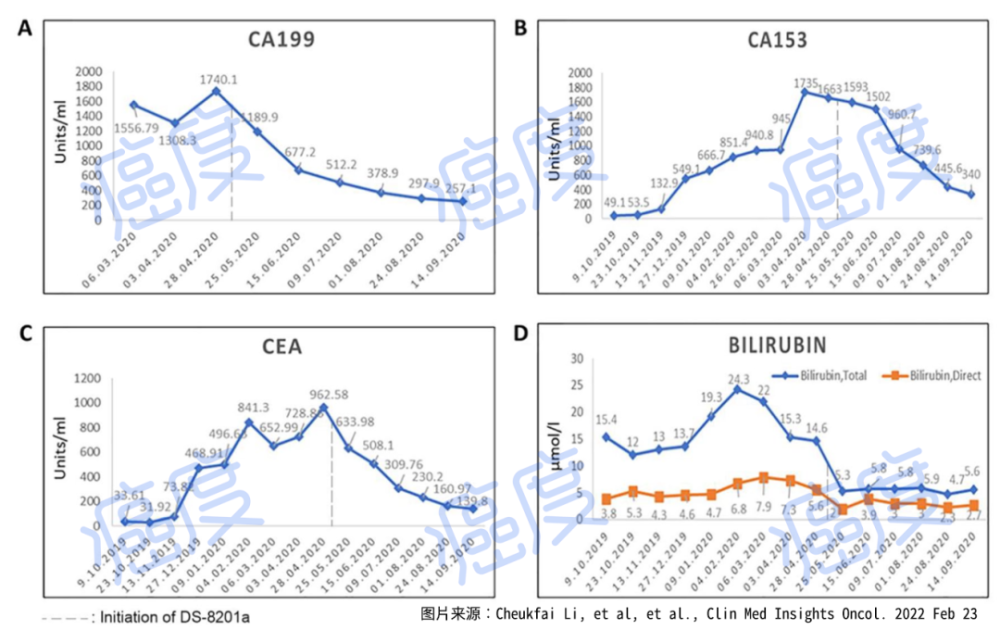 Figure 3. Changes in tumor markers and bilirubin during treatment
Figure 3. Changes in tumor markers and bilirubin during treatment
Inspiration: HER2 targets that need attention
Immunohistochemical test results of breast cancer patients should not be absolute, because some objective factors, such as sampling problems, may affect the accuracy of the results, and the expression of HER2 may vary with There are certain changes with the development of the disease. Therefore, in the course of treatment, you should communicate with your doctor in time and re-test at an appropriate time. If you find positive or low expression of HER2, you may benefit from DS-8201a.
The patient in this case sighs and wonders if she would have had a different outcome if she had been treated with DS-8201a earlier.
The fight against cancer is a long and hard battle. I just hope that there will be more new drugs and new treatment strategies in the future, so that we can stay away from cancer and embrace health.