At 12:00 a.m. on April 26th, Zhang Qi, director of the Cardiology Department of Shanghai Dongfang Hospital, rang, and another patient with myocardial infarction came. “Do emergency surgery right now!” With the call, he hung up the phone, and the medical staff on duty at the Cardiovascular Intervention Center of Dongfang Hospital immediately entered a “fighting” state. Masks, protective clothing, face shields, lead clothing, surgical gowns, etc. should be worn layer by layer, and surgical instruments and items should be prepared in place.
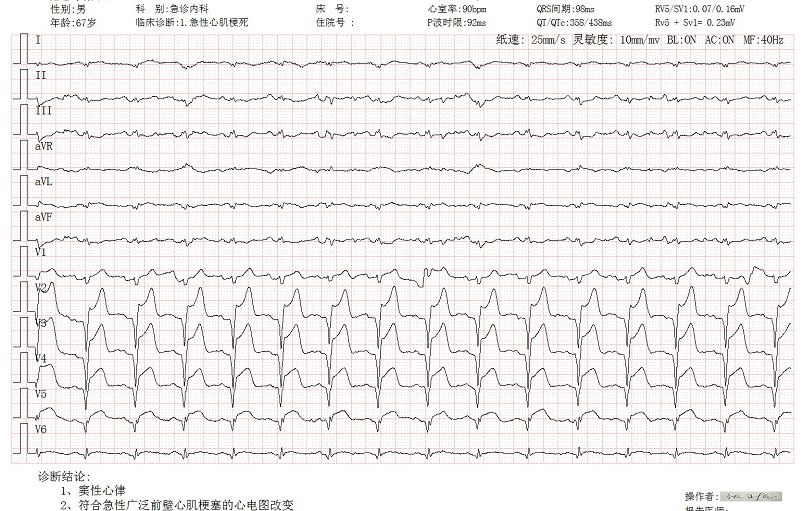
The patient this time is a 67-year-old male who just came home from the shelter that day. I had chest pains, and I was afraid of going to the hospital. When he arrived at the hospital, the patient had already begun to suffer from an unstable state such as lack of energy and low blood pressure. The electrocardiogram showed “extensive anterior myocardial infarction”. After consultation with the Cardiology Department, the fast track for myocardial infarction treatment was started immediately.
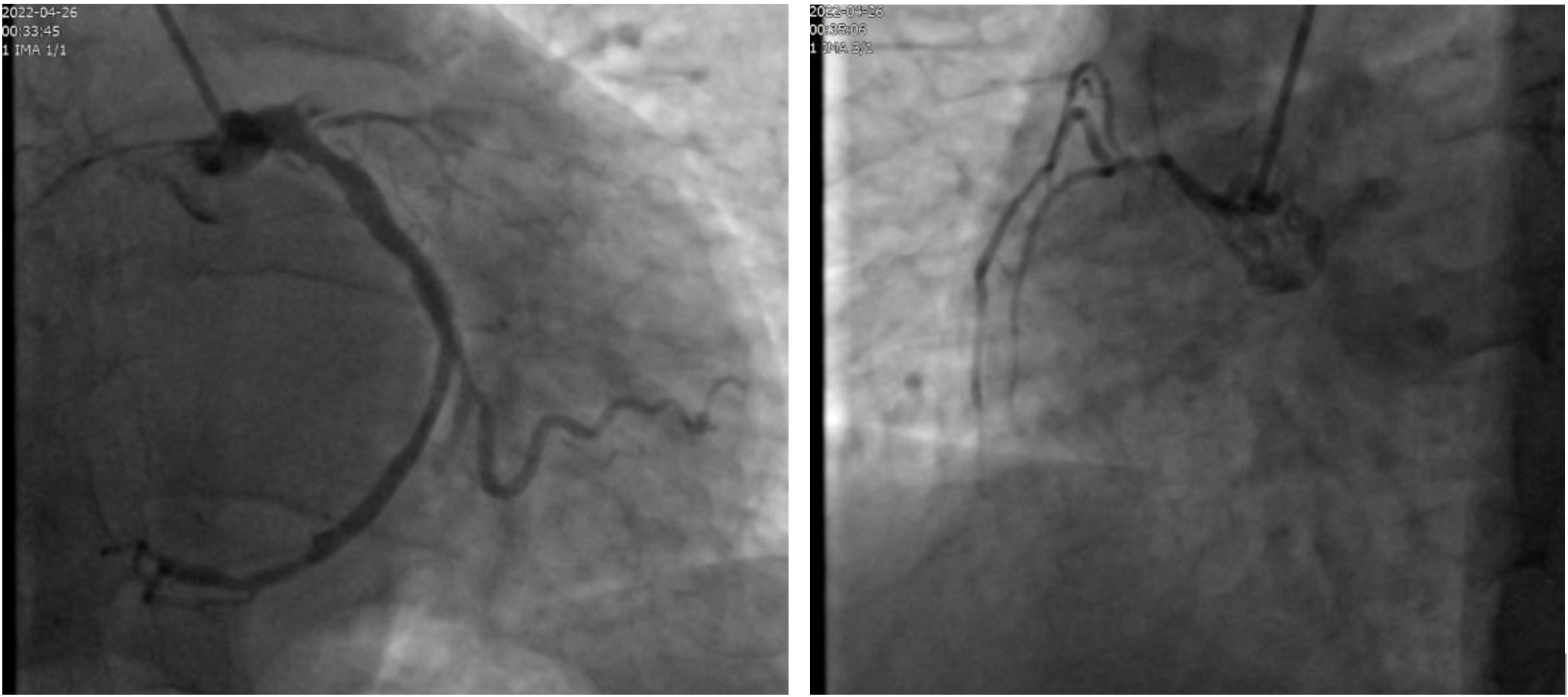
Results of emergency coronary angiography: initial occlusion of the anterior descending artery, massive thrombus, occlusion of the distal branch of the circumflex artery; small right coronary artery< /p>
After the angiography, Zhang Qi immediately realized that the problem was much more serious than he imagined. The opening of the anterior descending branch with the largest blood supply among the three major coronary arteries is completely occluded and contains a large number of thrombi; a large branch at the distal end of the circumflex artery tends to be occluded; the right coronary artery is relatively unobstructed, but congenitally small , has little effect on the overall blood supply.
Complete occlusion of the anterior descending artery is the main culprit for this myocardial infarction, but if the thrombus falls to the adjacent circumflex artery during the opening process, it will cause aggravation of circumflex artery ischemia or even acute occlusion . For this patient, the circumflex branch is the key to his life. If the circumflex branch is involved during the treatment, it is extremely fatal to the patient.
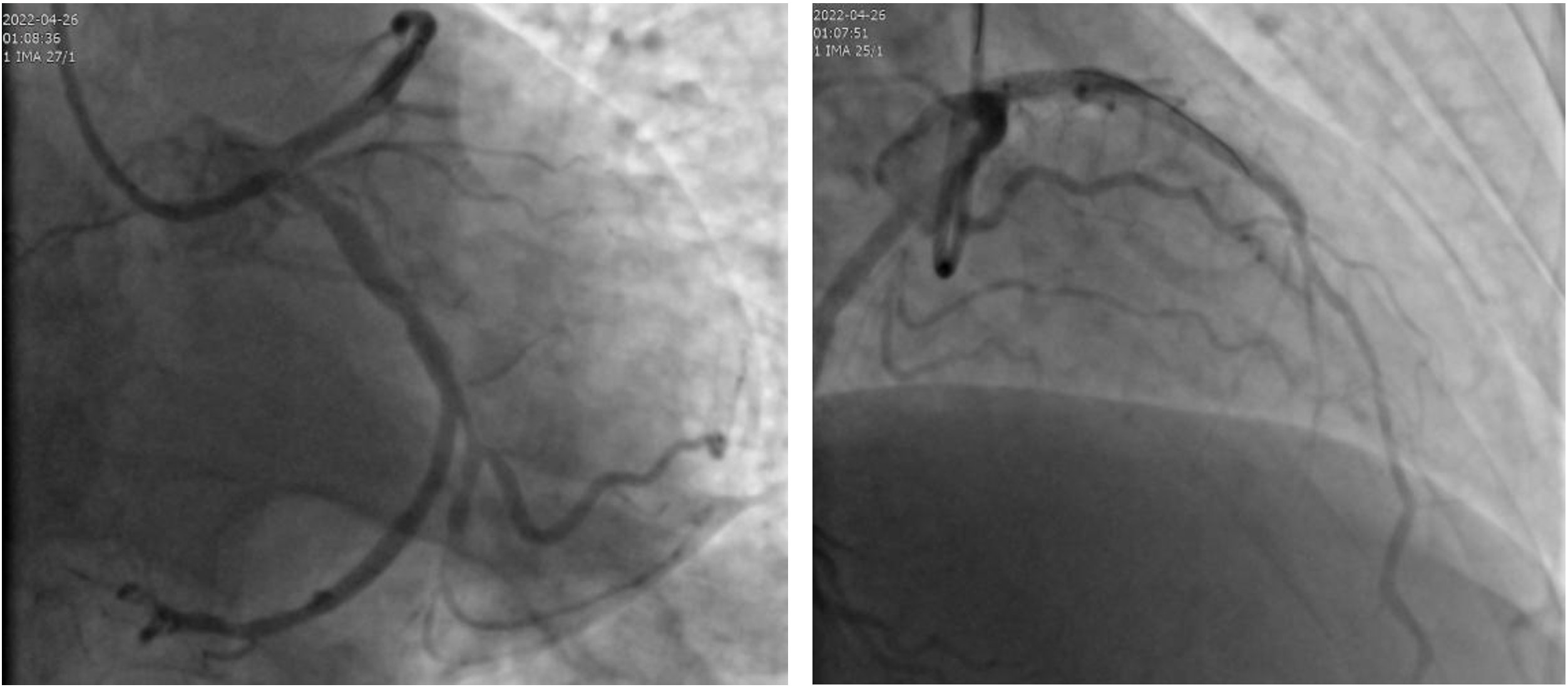
After emergency interventional treatment: stent implantation in the anterior descending branch, balloon dilation at the distal end of the circumflex branch, and blood flow recovery in each blood vessel
While communicating with his family about his condition, Zhang Qi and Guo Wei, who was operating together on the same stage, discussed the countermeasures for various situations, and the nurses have also prepared the aortic balloon counterpulsation pump, rescue medicines, etc. Subsequent interventional treatment was a near miss, the guide wire protected the circumflex branch, and the steps of thrombus aspiration, balloon dilation, and stent implantation in the occlusive lesions of the anterior descending branch were successfully completed. The balloon dilatation can better restore the overall blood supply state of the heart.
In more than 30 minutes, the emergency team of the Cardiology Department of Dongfang Hospital completed the whole process from preparation to interventional treatment. The patient’s symptoms were significantly relieved after the operation, and the blood pressure and heart rate also tended to be stable. A series of tasks such as escorting patients to the intensive care unit, sterilization of the catheterization room, and rearranging personnel were carried out in an orderly manner.
In the morning, during the ward round, the patient reported that the situation was much better than yesterday. But on the other hand, due to the huge blood supply area of the patient’s occluded blood vessels, the delay at home is also long. Although the occluded blood vessels were quickly opened after arriving at the hospital, the blow to his heart was still huge, and the risk of follow-up problems was still great.

Emergency interventional treatment under secondary protection
Zhang Qi carefully reviewed the patient’s various items. As a result of the inspection, the follow-up drug treatment plan was formulated together with the bed doctor. It was noon. When I turned on the mobile phone to read the news, several pieces of distressing news came into view. The deputy chief engineer of the large aircraft passed away due to a myocardial infarction, and was 33 years old in the epidemic report of the deaths were sudden cardiac death.
“This is not an isolated case.” Zhang Qi mentioned that, taking the Cardiovascular Department of Dongfang Hospital as an example, during the recent lockdown period, most of the myocardial infarction patients admitted to the department were at home or at home. Those who were “excluded” in the unit isolation for a long time, or even a few days, came to the hospital to see a doctor. In fact, the Cardiology Department of the two hospital districts of Dongfang Hospital has always been equipped with a 24-hour standby team to respond to critically ill patients at any time. Since the outbreak in early March, the wards and general wards of the department have maintained relatively independent operations, and doctors in each ward have implemented a closed-loop work system. Among them, several doctors in the intensive care unit have been sticking to their posts for more than a month and have never returned home.
“During the lockdown period, activities decreased, anxiety increased, and bad habits such as staying up late and smoking were even worse. These have important effects on the cardiovascular system.” Zhang Qi reminded: “Whether it is accompanied by People with chronic diseases, or middle-aged and young people, if they have chest tightness, chest pain and other uncomfortable symptoms, they must pay great attention to it, go to the hospital for examination as soon as possible, and don’t ‘abandon’.”