For medical professionals only
Behind a professional image, there is never a colorful landscape.
What do you think of MSF frontline workers? Always motivated and ready to save lives? Perhaps many people, including themselves, hold such expectations. However, frontline workers are not always so strong. In the face of patient deaths, medical equipment and treatment options, they also accumulate stress and negative emotions that keep them from being at their best all the time. The COVID-19 pandemic has given us an opportunity to discover more true stories and to learn more about the people who stand on the front lines of medical care around the world, seemingly fearlessly carrying out all their rescue missions.
Looking back, the professional image was never full of colorful scenery.
A heartbreak is a life-and-death decision

Dr Koana Rojas is a pediatrician from Venezuela. In 2020, she chose to join the MSF team, working in a Covid-19 ward in Caracas. ©MSF
Dr. Rojas remembers that one of her patients was a 40-year-old pediatrician. He was admitted to the hospital with a confirmed case of Covid-19. In the beginning, he had difficulty breathing and the only thing that could help him was to go to the ICU (intensive intensive care unit). But the hospital beds were full at the time. In the end, Dr. Roxas had to put him on palliative care, and the patient died soon after.
“I’ve only seen paediatric patients for 7 years, and now I’m dealing with adults, which is beyond me. Palliative care means there’s nothing we can do…we can’t give him what he needs I watched his heartbeat gradually slow down, he lost consciousness, and then died.” Dr. Rojas still couldn’t help choking when he recalled, “The thought that I might be him too… It’s too hard. I Remember, his son comforted me when he was desperate, ‘Don’t worry, doctor, I know you tried your best.’ I couldn’t look him in the eye. Deep down, I knew there was still something to do, such as sending him off to the ICU.”
Dr. Roxas would like to spend as much time with him as possible if he were to go back in time. “I know his days are running out, and he knows that, which makes me want to do more for him, like showing him family videos, or chatting with him so he doesn’t feel alone.”
Healing is a journey of dialogue with the Self. Following the advice of MSF psychologists, Dr. Rojas named her emotions one by one, teasing everything out to find the problem. “Connecting with nature helps me overcome these conditions, a flower, a pine tree… close my eyes, savor all the smells, and be in it, I can let go of it all, like breathing, and tell me what will happen Okay, tomorrow is another day.”
Painful, misunderstood

Manqoba Sikhondze is a MSF home care nurse in Swaziland. ©MSF
Hironze is working on a home care team in Swaziland during the COVID-19 outbreak. At that time, he kept receiving calls for help from different parts of the district, most of them were elderly and critically ill patients who were suffering from other diseases at the same time. As a medical staff, he has to travel around the clock to different places for medical treatment. Unfortunately, due to the lack of resources during the epidemic, Xi Hongze has to make difficult decisions from time to time, such as which patient to treat first. However, not everyone is aware of their limitations, and even some patients and family members may misunderstand them and stand by.
“A family member said that he knew that medical staff could get more pay for night shifts, so he misunderstood that we came at night on purpose. In fact, we have always only had a fixed salary, and this arrangement is completely irrelevant. Subsidies. It’s really hard for me to say that. It’s hard for people to understand, some of the difficulties stem from structural issues. It’s not the medical team’s fault, many things are beyond our control, but we’re on the front lines The staff of the people are the people that the public can directly contact, and as a result, their anger, dissatisfaction and various emotions are often only vented to us.”
Xi Hongze also sometimes thinks about those he can’t help, “Although it is very painful, I will re-examine, if we make different arrangements or decisions, the patient said Maybe there is a chance to survive?”
Torment is separation from love

Marisela Douaihy is an ICU physician in Venezuela. ©MSF
The COVID-19 pandemic has had an unprecedented impact on much international humanitarian work, and staff involved have to juggle and adapt to changes in their personal lives outside of work, and are constantly faced with choices. E.gIn response to border closures or entry and exit restrictions in various countries, they need to consider whether they should continue to stay at the location of the mission, or go home to reunite with their families and help their own countries.
“COVID-19 is different from other diseases in that, once diagnosed, anyone can need intensive care, but the reality is that we don’t have enough beds to keep all Venezuelans in hospital. When you There are 15 equally serious patients in front of you, who do you choose to save?”
Dr. Duaixi admitted that she felt like she was suffocating when she saw those who were barely breathing. “Such a catastrophe is so heart-wrenching. Everyone’s begging me for help, but there’s nothing I can do. As an ICU doctor, I’m used to facing death, but it’s still unacceptable that 10 or more patients died in the same day. .The pain of being helpless and saying to 10 families a day ‘We’ve done everything we can, but I’m sorry, there’s nothing I can do about your family.’, this feeling of helplessness, made me start counseling with a psychologist.”
Speaking of family, the most effective encouragement for Dr. Duais is always from them. However, since she has to work in a high-risk location, in order to prevent her family members from having the chance to get sick because of her, she has to be isolated from them, which makes her seem to be at a loss in difficult times. “It’s really hard not being able to see my family. I haven’t hugged my daughter for a year.” She couldn’t help crying.
The hard part is accepting giving up
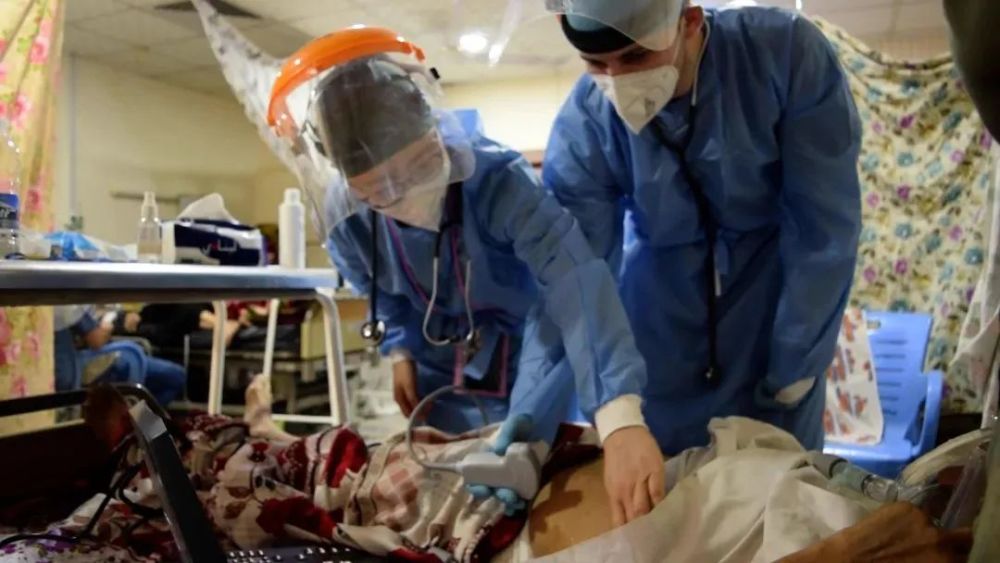
Liu Yiyun (left), an ICU doctor from Shanghai, joined MSF’s COVID-19 treatment project in Iraq in October 2020. ©Ghada Safaan/MSF
At the height of the outbreak in Baghdad. MSF provides support at the local teaching hospital, Al-Kindi Hospital, to help treat critically ill and critically ill patients. The beds in the hospital are always full, but there are only 3 large non-invasive ventilators. Tracheal intubation is a very common operation in the ICU, but the local government stipulates that intubation of patients with new coronary pneumonia is not allowed, and the treatment measures are very limited.
Liu Yiyun remembers that a grandmother in her 70s was treated in the ward for a period of time. Her family members are very kind, not only taking care of the elderly, but also helping to take care of other patients. With the efforts of the medical staff and family members, the condition of the grandmother improved for a while, but suddenly one day, the patient suddenly fainted. Liu Yiyun and several doctors and nurses rushed to the bedside and found that the patient had cardiac and respiratory arrest. Cardiopulmonary resuscitation didn’t help. When the rescue equipment was withdrawn, the whole family was beside the hospital bed and surrounded the old man, crying.
“At first, I wanted to discuss the cause of the patient’s death with the local doctor, but I couldn’t go on after a few words. I turned around and walked to an empty corner outside the ward, and my tears fell instantly. I can’t touch my hands, I can’t wipe my eyes, I don’t have tissues, and the mask is very precious. I can only stand there for two or three minutes and wait for the tears to dry before returning to the ward.” Thinking of the experience a year ago, Liu Yiyun is still emotional .
“Although I have worked in the ICU for many years, I have never seen so many life and death in a short period of time. When the patient’s hope is low, the eyes of the local doctors are on me, I know Everyone wants to save the patient, but I also know that continuing to give the patient the highest intensity of treatment will not change the outcome, but will only increase the patient’s suffering. However, ‘giving up’ is never easy. I always think , the time when the doctor gives up is when the patient truly loses hope of treatment, so it is a big challenge for me to choose to give up high-intensity treatment to palliative care.”
This seems to be a common problem for doctors – taking patients who are rescued for granted, and being bitter about patients who can’t be rescued. During the 4 months on the project, this kind of brooding emotion always haunted Liu Yiyun. But that is, in the past 4 months, with the efforts of everyone, the mortality rate of severe and critically ill patients has dropped from nearly 100% to 80%, and then to 60%. These changes gave Liu Yiyun some comfort.
Maintaining mental health is important for everyone. Working on the front lines for months, staff are often tired and have many new experiences to reflect on. They may need assistance so that they can better deal with their emotions and natural responses to traumatic experiences. Before embarking on the mission, they undergo comprehensive preparatory training, including a mental health component. In addition, each operational unit has a mental health support group that encourages all frontline staff to reach out for help, and if the team experiences a traumatic event or an unusually high-pressure state, the organization’s psychologists will travel to the project site or connect via phone or video as appropriate. line support.
Source: MSF
Editor in charge: Tian Dongliang
Hot text recommendations



* The medical community strives for the accuracy and reliability of its published content when it is reviewed and approved, but does not regard the timeliness of the published content, and the accuracy and completeness of the cited materials (if any), etc. Make any promises and guarantees, and do not assume any responsibility for the outdated content, possible inaccuracies or incompleteness of the cited information. Relevant parties are requested to check separately when adopting or using it as a basis for decision-making.