Written by Wang Wei | Editor-in-Chief | Zhou Yebin
Osteosarcoma is the most common primary malignant bone tumor in children. About 40-50% of patients can recur or develop distant metastasis after surgery, resulting in a 5-year survival rate of less than 30%. Adriamycin is currently one of the first-line chemotherapy drugs for osteosarcoma, but its clinical application is limited due to its high metabolic rate, low osteosarcoma affinity, high cardiotoxicity, bone marrow suppression and other toxic side effects. How to increase the intratumoral enrichment of doxorubicin and improve the prognosis of patients is still an urgent problem to be solved in the clinical treatment of pediatric osteosarcoma.
August 31, 2022, published in Journal of Controlled Release titled IL-11Rα-targeted nanostrategy by the joint team of Soochow University and Beijing Jishuitan Hospital Empowers chemotherapy of relapsed and patient-derived osteosarcoma article, Researchers have synthesized IL-11 ligand-functionalized redox sensitive Multimeric nanoparticles, which can encapsulate doxorubicin to reduce its side effects and at the same time promote intratumoral enrichment of the drug, provide a new drug delivery method for clinical chemotherapy of osteosarcoma.

In recent years, researchers have developed a variety of nano-drug delivery systems to improve the clinical efficacy of chemotherapy drugs in osteosarcoma, including bisphosphonates, hyaluronic acid, folic acid, peptides, etc. However, Such synthetic drugs often fail to specifically bind osteosarcoma cells. In this study, it was found that IL-11Rα receptors were highly expressed on the surface of tumor cell membranes in osteosarcoma tissue specimens. Therefore, the researchers linked its ligand IL-11 to nanopolymers through an amide addition reaction, and self-assembled to synthesize redox IL11-PDox, a sensitive delivery carrier for doxorubicin, The polymer has small particle size (33nm), strong stability and controllable drug release. In a non-redox environment, less than 10% of the drug was released from the polymer, while under glutathione stimulation, about 86% of the total drug was released in 12 hours.
In addition, researchers found that IL11-PDox enhanced the endocytosis of doxorubicin in osteosarcoma cells. Compared with free doxorubicin, the endocytosis of doxorubicin in osteosarcoma cells in IL11-PDox group was significantly increased by 3.7 times by flow cytometry. CLSM imaging more intuitively observed that doxorubicin in the IL11-PDox group entered cells rapidly within 4 hours, and was transported into the nucleus from the cytoplasm.
In vitro cell experiments found that IL11-PDox had stronger cytotoxicity and inhibited migration ability. MTT assay found that the IC50 of IL11-PDox in osteosarcoma cells was only 0.05ug/ml, while the IC50 of free doxorubicin was 9.6 times that of IL11-PDox; flow cytometry showed that IL11-PDox induced 84.6% Osteosarcoma cells were apoptotic, while free doxorubicin was only 47.2%; in addition, IL11-PDox could more significantly inhibit the colony formation and cell migration ability of tumor cells.
Subsequently, in order to further explore the in vivo efficacy of IL11-PDox, the researchers established 3 mouse osteosarcoma models, including osteosarcoma orthotopic tibia model, osteosarcoma postoperative recurrence with lung Metastasis model and human tumor xenograft (PDX) model, based on the three models, the researchers focused on verifying the in vivo targeting and anti-tumor effects of IL11-PDox.
The researchers found that IL11-PDox could target and accumulate in orthotopic osteosarcoma of the mouse tibia, and significantly inhibited its growth. 4 hours after IL11-PDox was injected into the tail vein, it was observed that doxorubicin rapidly accumulated to the tibial tumor site, while the distribution of other organs in the body was very small; IL11-PDox effectively inhibited tumor growth, and 3/5 of the mice tumors were treated for 30 days. At the same time, IL11-PDox reduced the organ toxicity and side effects of doxorubicin, and the median survival time was significantly prolonged to 74 days. In general, it showed stronger superiority than free doxorubicin.
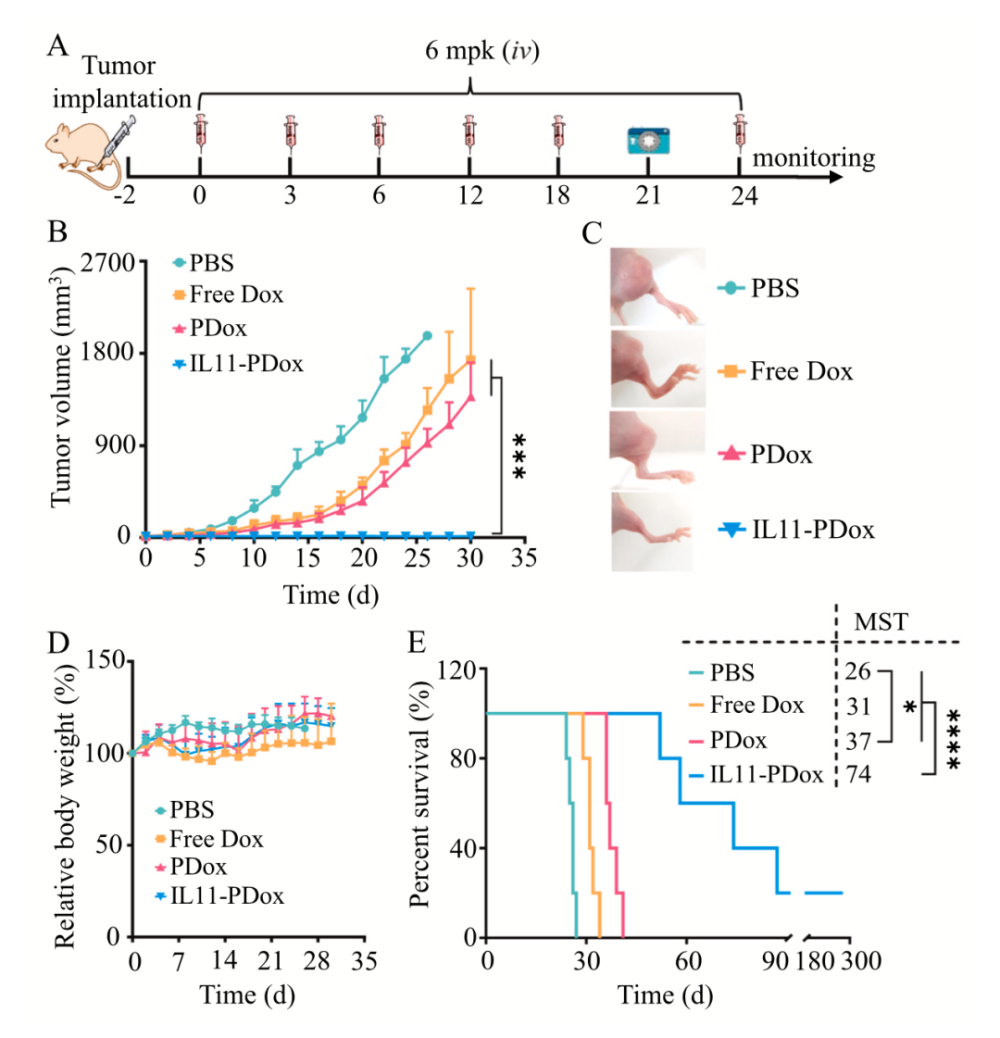
The efficacy of IL11-PDox on orthotopic osteosarcoma of the tibia in nude mice. (A) Workflow: Tumor cells were seeded 2 days in advance, and mice were treated with free doxorubicin Dox, polymer-encapsulated doxorubicin PDox, and IL11-PDox on days 0, 3, 6, 12, 18, and 24, respectively. (B) Tumor growth curve (C) Pictures of mouse hind legs on day 21 (D) mouse body weight change and (E) Kaplan-Meier survival curve.
The researchers then used a mouse model of osteosarcoma recurrence after surgery, and found that postoperative use of IL11-PDox significantly inhibited the recurrence and lung metastasis of osteosarcoma. Compared with free doxorubicin that only limited tumor growth in the early postoperative period, uncontrolled tumor growth and multiple lung metastases in late stage, IL11-PDox can completely inhibit the in situ recurrence of osteosarcoma in mice, and the lung tissue and No tumor cells were observed in lymph node histology. Molecular mechanism studies found that IL11-PDox can promote apoptosis by reducing the expression of Bcl-2, inhibit the proliferation of AKT, and reduce the phosphorylation of STAT3 to inhibit the metastasis of tumor cells.
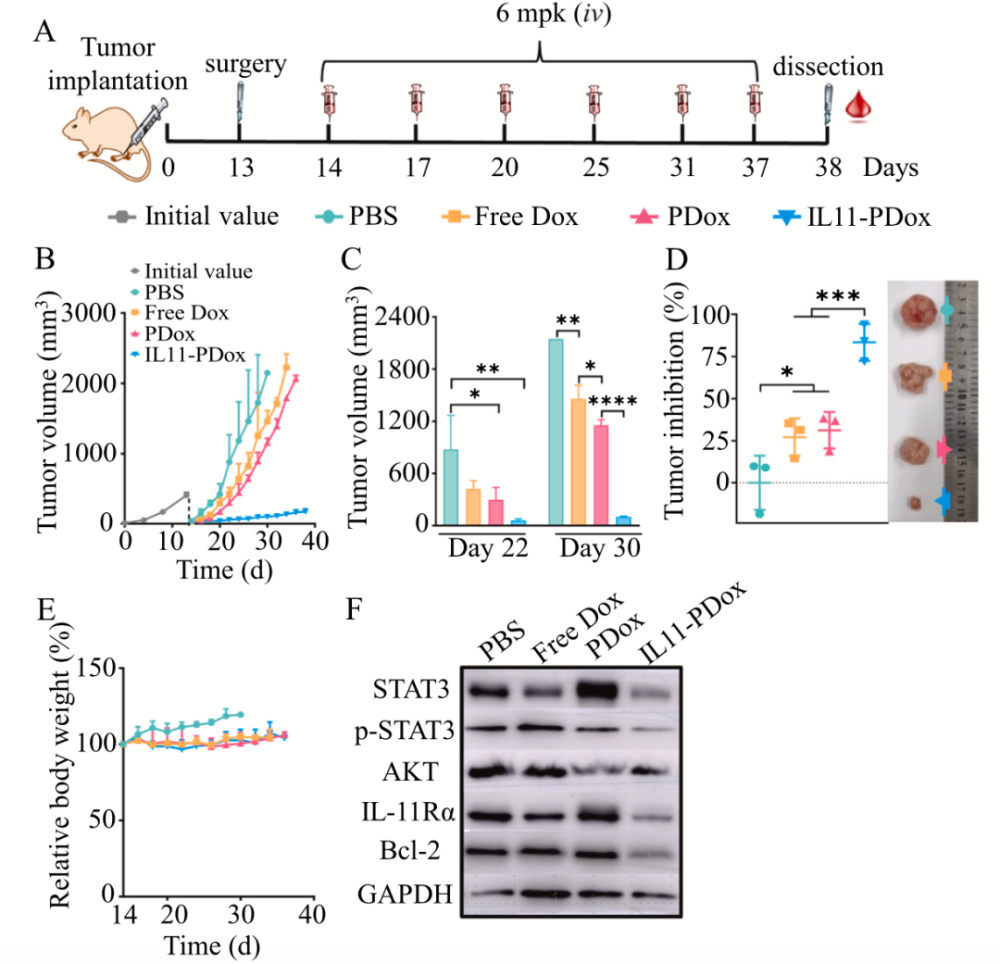
The efficacy of IL11-PDox on postoperative recurrent osteosarcoma in nude mice. (A) Workflow: Recurrent osteosarcoma model was established by surgical resection of tumor and treated with IL11-PDox, PDox, free Dox on days 14, 17, 20, 25, 31 and 37 (B) Tumor growth curve ( C) Tumor volume on days 22 and 30 (D) Tumor inhibition rate and photographs of isolated tumors (E) Body weight change in mice (F) Bcl-2, IL-11Rα, AKT, STAT3 and p in tumors on day 38 – Expression of STAT3.
Finally, the researchers found that IL11-PDox also has a strong anti-tumor effect in the mouse PDX osteosarcoma model. The tumor inhibition rate (TIR) of IL11-PDox on osteosarcoma PDX can reach 80%, while that of free doxorubicin is only 40%; H&E staining showed that intratumoral tumor cells were significantly reduced and apoptotic after IL11-PDox treatment cells increased significantly.
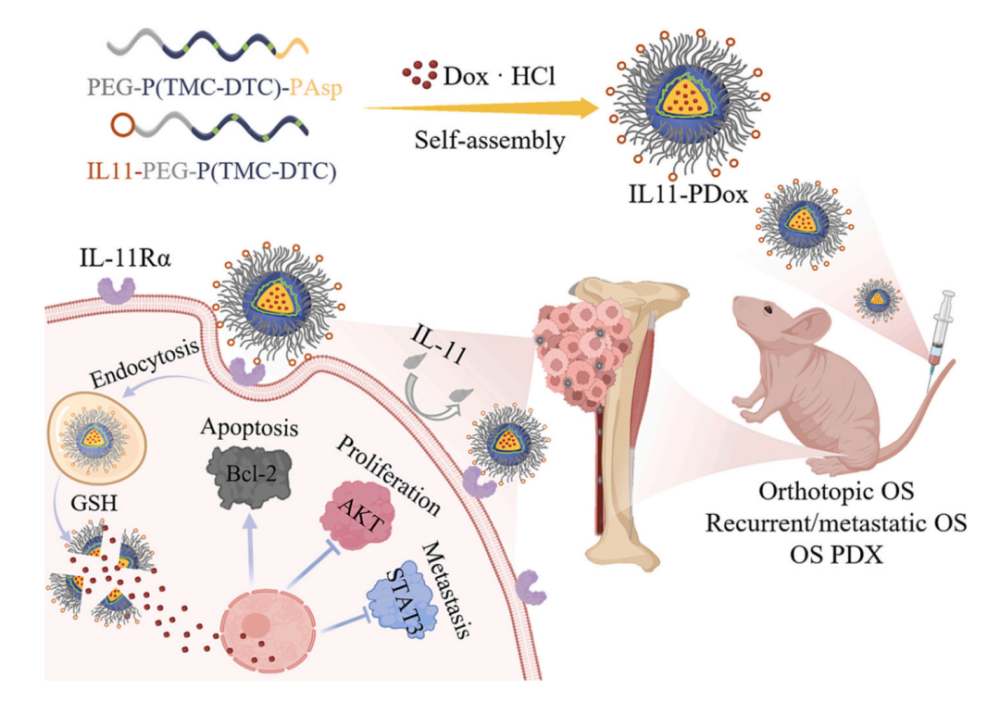
In conclusion, compared with free doxorubicin,the IL11-PDox nano-drug delivery system established in this study has unique advantages, including small size, high specificity, and low toxicity Side effects, good stability, redox reactivity, and ease of manufacture. The vector greatly improves the osteosarcoma targeting and antitumor efficacy of doxorubicin, and shows excellent inhibitory effects in osteosarcoma orthotopic models, tumor recurrence and lung metastasis models after surgical resection, and PDX models. The clinical treatment of osteosarcoma in children provides a very promising therapeutic strategy.
Writing

Editor

Production
Typesetting | Sheila proofreading | uu