1. What is TAVR surgery?
The so-called TAVR, the Chinese name is translated into: Transcatheter Aortic Valve Replacement (TAVR, Transcatheter Aortic Valve Replacement), and it is also translated into TAVI surgery, the content of the two expressions is consistent. The procedure is to use intraluminal catheter technology to load the artificial valve into the catheter system, and deliver the artificial valve to the aortic valve position through the peripheral blood vessel or the apical approach to release and replace the diseased valve.
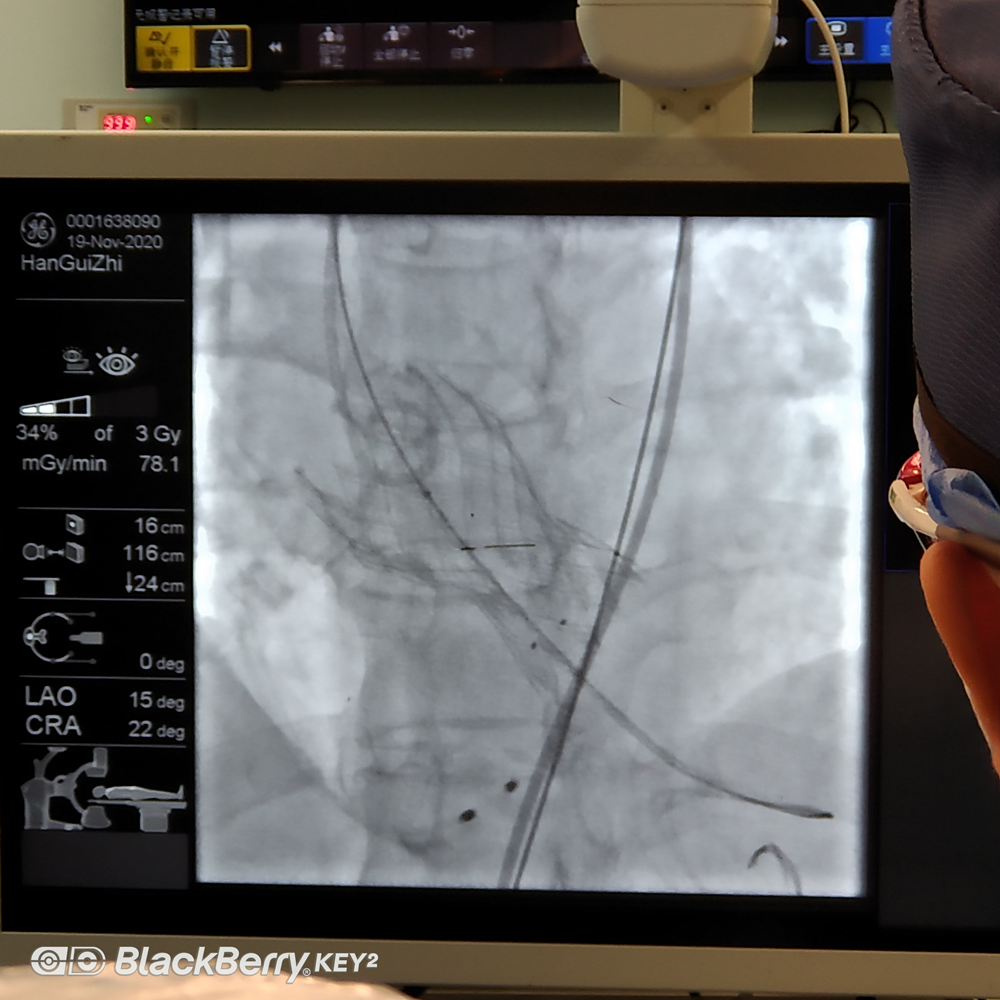
2. What kind of patients are suitable for TAVR?
TAVR was first reported in the world in 2002. It was introduced in China around 2012. At that time, there were only 4 single centers in China that could perform operations independently. The number of single centers exceeded 100 for the first time. As of 2022, according to reports, there are more than 400 single centers in China that can perform operations independently.
According to the ACC/AHA guidelines (American College of Cardiology), TAVR is the first choice for aortic valve replacement in high-risk patients who cannot tolerate surgical treatment or have high surgical risks . For example: elderly patients (patients older than 80 years old recommended by foreign guidelines); patients with long related medical history and poor cardiac function; patients with many medical complications, such as diabetes, pulmonary insufficiency, renal insufficiency, digestive tract diseases, etc. Patients with comorbidities; patients who have undergone thoracotomy before and need to undergo cardiac surgery again this time can choose TAVR surgery to replace the aortic valve.
3. What are the advantages of TAVR over traditional thoracotomy aortic valve replacement?
Compared with traditional thoracotomy under cardiopulmonary bypass, TAVR surgery eliminates the need for median thoracotomy in traditional aortic valve replacement surgery. Steps such as beating and rebeating of the heart reduce the surgical trauma of the patient and greatly reduce the risk of surgery. Postoperatively, the patient will not have a large surgical wound from the suprasternal fossa to the xiphoid process like the traditional thoracotomy, and there will be no postoperative pain after the sternum. Generally, there is only a puncture point in the groin on one or both sides. Compared with traditional thoracotomy aortic valve replacement, TAVR surgery has relatively shorter anesthesia time and operation time, and the overall time for patients is usually completed within 120-150 minutes. The patient feels good after the operation. Generally, he can get out of bed 24 hours after the operation. He is hospitalized for 3 days after the operation, and the review is normal, and he can be discharged from the hospital.
4. What is the lifespan of the TAVR valve?
At present, the valves used in TAVR surgery are all biological valves. The currently internationally recognized gold standard is the bovine pericardial valve produced by Edwards. According to current reports, the service life of the bioprosthetic valve is generally 10-15 years after the operation, after which the bioprosthetic valve may show calcification damage. According to the clinical situation, stenosis or (and) insufficiency may occur, and the damage can be replaced by the minimally invasive TAVR surgery again. the aortic valve.

5. The patient needs to undergo TAVR surgery. When choosing the valve, which one is imported or domestic?
At present, my country’s domestic TAVR valves approved by the CFDA for clinical application are all valve products with independent intellectual property rights in China. The clinical test results are not significantly different from similar foreign products. There is the world’s only TAVR valve approved for aortic regurgitation, and it is also used abroad.
6. Anesthesia methods and options for TAVR surgery?
At present, there are three methods of anesthesia for TAVR surgery in China:
1) General anesthesia for endotracheal intubation;
2) Non-intubated general anesthesia (local anesthesia + enhanced MAC);
3) Local anesthesia monitoring.
If a patient needs to undergo TAVR surgery, the anesthesiologist should fully evaluate the patient’s past medical history, general condition, current medical history and medical comorbidities before surgery, and choose the most suitable anesthesia method for the patient. Regardless of the choice of any of the three anesthesia methods, the single-center experience of the Anesthesia Center of Beijing Anzhen Hospital also requires general anesthesia for tracheal intubation to prepare anesthesia options for patients to prevent intraoperative accidents.
7. Taking the TAVR operation under general anesthesia under tracheal intubation as an example, what should we do as anesthesiologists after the patient enters the room?
1) First of all, we should fully communicate and educate the patients, eliminate or reduce the anxiety and fear of the patients, and obtain the trust and cooperation of the patients;
2) Give the patient five-lead ECG monitoring, blood oxygen monitoring, assess the patient’s preoperative ECG status, closely monitor various vital signs, and perform invasive upper limb surgery for the patient under local anesthesia. Blood pressure monitoring and venous indwelling needle placement to maintain fluid support with an effective flow rate and keep the patient warm;
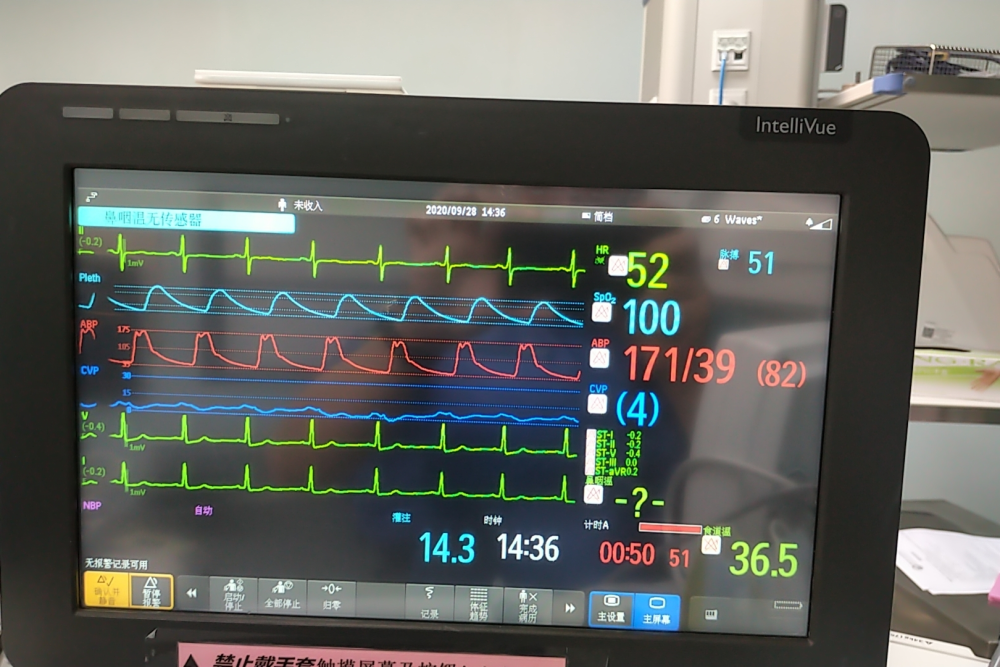
3) Re-evaluate according to the condition, and consider the establishment of central venous access and monitoring of central venous pressure under local anesthesia before induction of anesthesia as appropriate;
4) After the central venous access is established, general anesthesia is induced. After the tracheal intubation is completed, it is properly fixed, and the vital signs of the patient are continuously monitored to maintain the stability of the depth of anesthesia and hemodynamics.
5) According to the patient’s condition, perform transesophageal/transthoracic echocardiography, and perform the last ultrasound diagnosis and condition assessment for the patient before surgery.
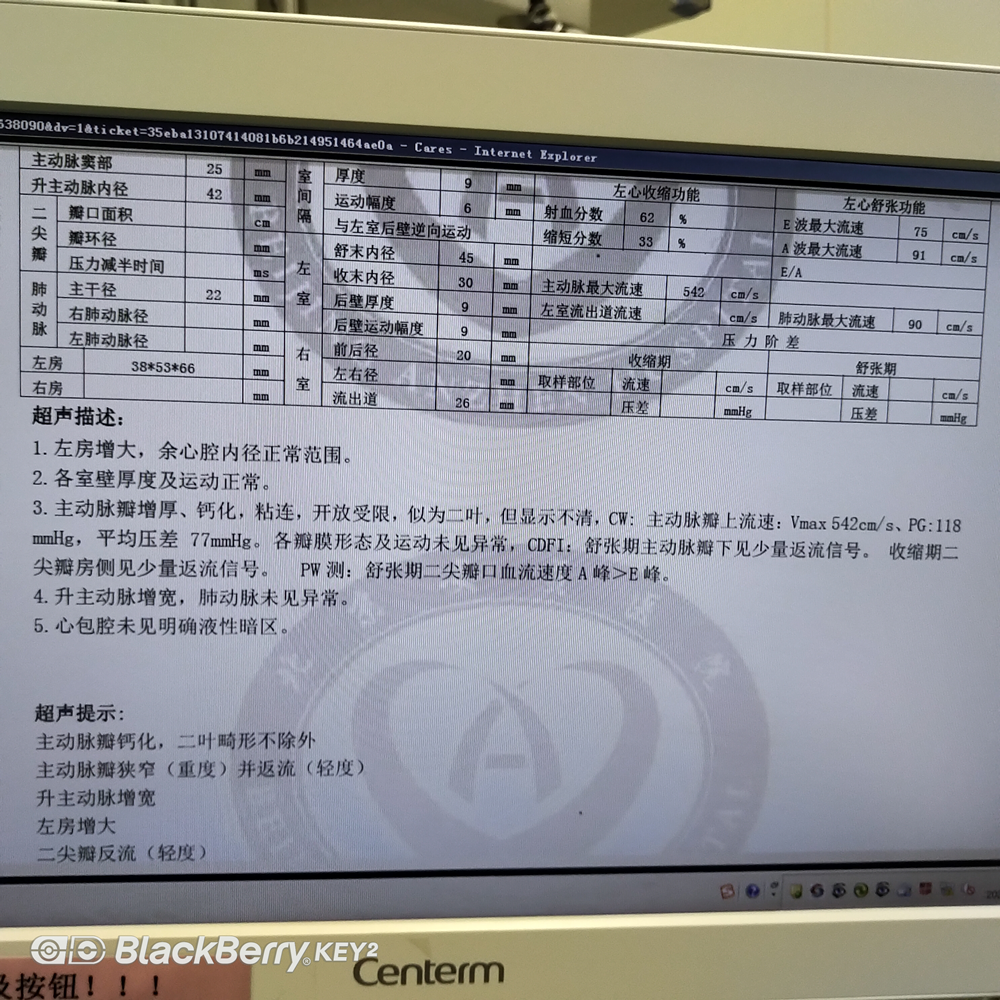
6) At the beginning of the operation, ACT > 300 seconds after heparinization, and after heparinization reaches the standard, the anesthesiologist needs to know the patient’s coronary condition and determine whether the patient needs a one-stop solution to the existence of coronary arteries question. The surgeon indwells a temporary pacemaker for the patient, confirms the electrode position of the temporary pacemaker, the pacing perception effect and the pacemaker parameter setting.
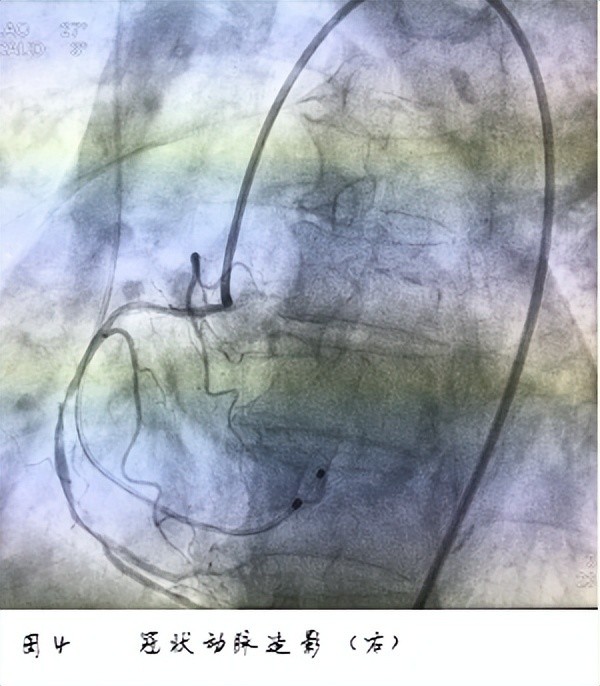
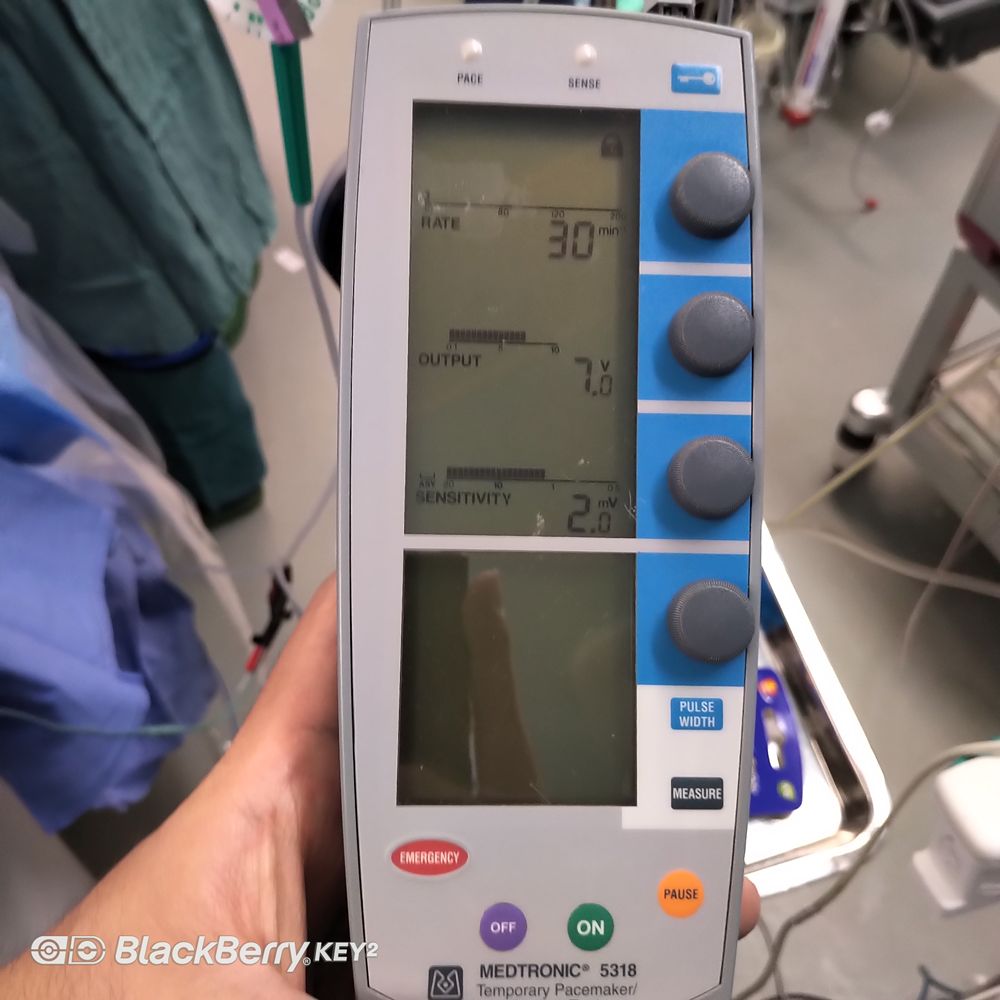
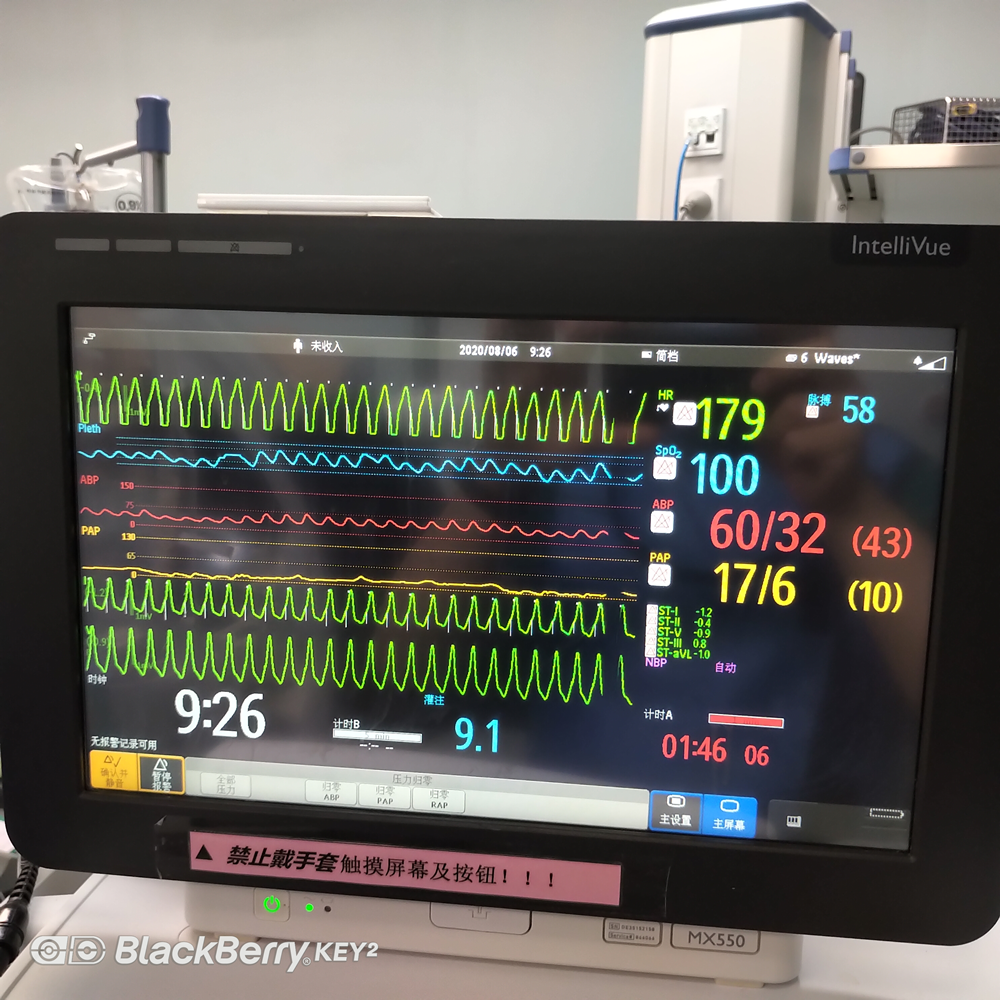
7) During the operation, when the surgeon performs operations such as expanding the valve, placing the valve, and expanding after placement, the patient must be treated with “overspeed pacing”, and the anesthesiologist should be strict Monitor vital signs. After the “overspeed pacing” is stopped, the patient’s ECG monitoring should be observed, whether there is a spontaneous heart rhythm on the ECG, and whether there is a rapid fatal arrhythmia, bundle branch block or conduction block. If a serious arrhythmia occurs , should be corrected in time.
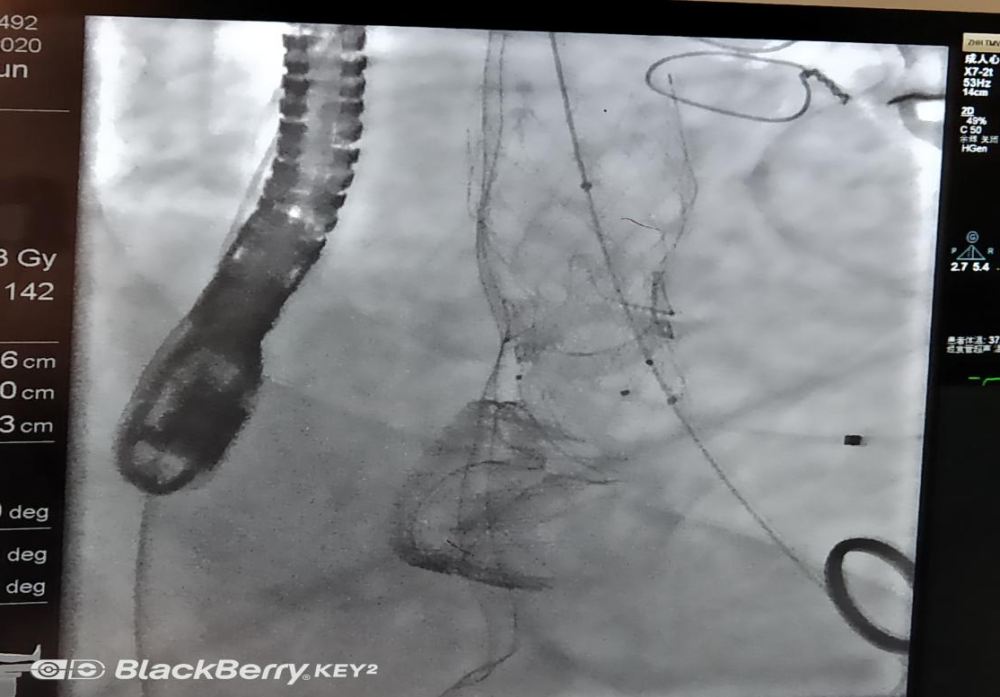
8) After the operation, the surgeon will evaluate the patient’s immediate postoperative effect according to the contrast image and echocardiography. If the surgical effect is satisfactory, the preparation for the recovery period from anesthesia and the suction device can be carried out. Aspirate the secretions from the patient’s trachea and oral cavity, closely monitor the patient’s vital signs, observe the patient’s anesthesia and recovery status, and the tracheal intubation can be removed if the evaluation criteria are met. After extubation, the patient’s general condition and vital signs should be closely monitored. Do a good job in dealing with the risks associated with the perioperative period.
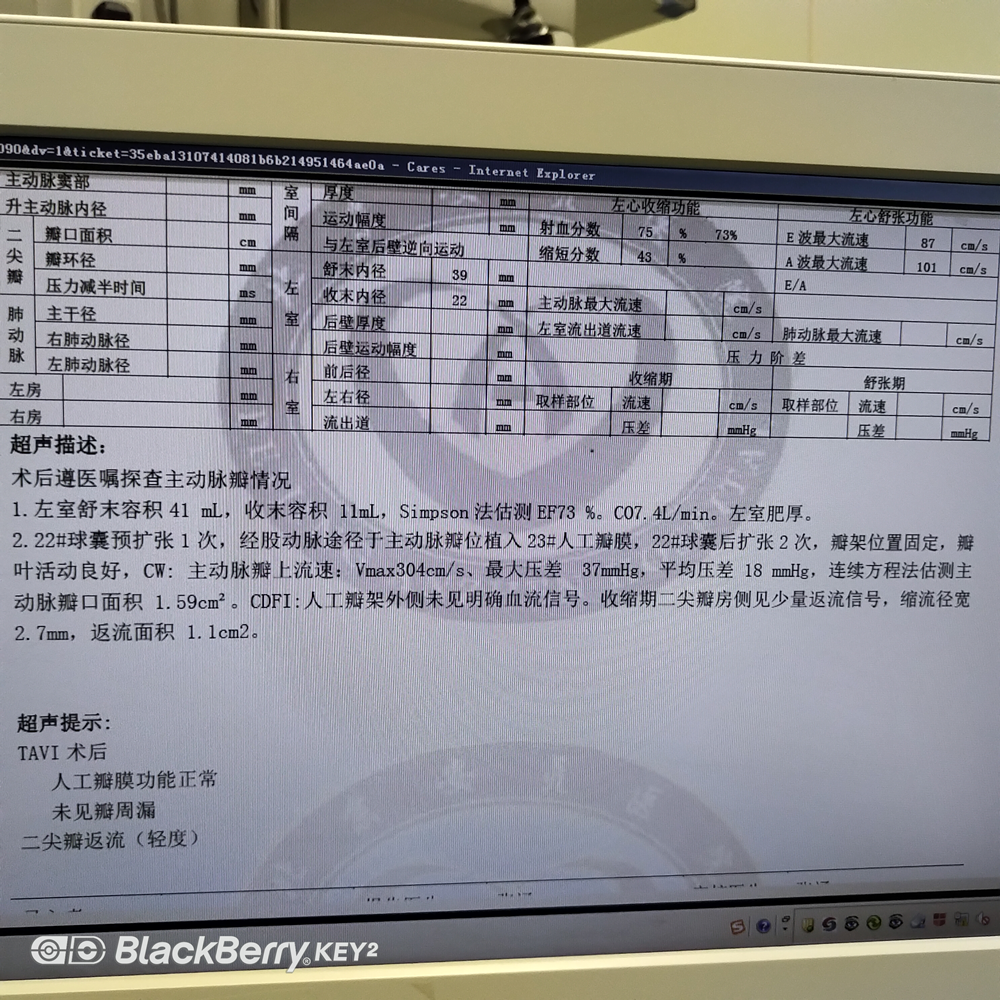
9) The patient’s general condition is good after surgery, and his vital signs are stable, and he can be transferred back to the intensive care unit for further treatment.
I believe that with the advancement of technology, the continuous accumulation of surgical experience, and the continuous efforts of all aspects of the team, a large number of patients will benefit from our work and improve their disease conditions. , life-enhancing therapy.

Author: Wang Jianyu, born in the 1980s in Beijing, was born in a medical family. He studied at China Union Medical College and now works in the Anesthesia Center of Beijing Anzhen Hospital.
[Warm reminder] Please pay attention, here are a lot of professional medical science, to reveal the secrets of surgical anesthesia for you~