I want to go to the toilet as soon as I drink water. Every time I urinate, but I only pee a little when I go to the toilet?
Frequent waking up badly affects sleep?
Many checks without any problems?
Then you may have Overactive Bladder!
What is overactive bladder? Let’s take a look below!
What is overactive bladder?
Overactive bladder (OAB) is a common disease in urology. The International Continence Society (ICS) defines overactive bladder as uric urgency Symptoms are the main manifestation, most of which are accompanied by frequency, with or without the clinical syndrome of urge incontinence, while excluding urinary tract infection or other obvious pathology Variety. It obviously affects the daily life and social activities of patients, and has become a major disease that plagues people.

Why do I get overactive bladder?
The cause of overactive bladder is unknown, but it is thought to be related to several factors:
01
Detrusor instability
Due to non-neurogenic factors, the abnormal contraction of the detrusor muscle during urine storage causes corresponding clinical symptoms
02
Neurogenic Theory
Abnormalities of central or peripheral nerves, especially bladder afferents, can lead to overactive bladder;
03
Myogenic Theory
The involuntary contraction of the detrusor muscle during urine storage causes corresponding clinical symptoms;
04
Allergic bladder
Desire to urinate occurs at small bladder capacity
05
Other reasons
Such as mental illness, abnormal hormone metabolism, inflammation, bladder outlet obstruction, application of drugs that affect bladder function, etc.
Symptoms of overactive bladder
Symptoms in typical cases include urgency, frequency, nocturia, and incontinence during urgency, the most common of which is urgency.
01
Urgency
Sudden and strong urge to urinate, it is difficult to subjectively suppress and delay urination.
02
Frequency urination
Patients feel that the frequency of urination is too frequent every day. The frequency of urination is more than 8 times during the day and no less than 2 times at night. When the urine volume is less than 200ml each time, it is considered as frequent urination.
03
Nocturia
Waking up to go to the bathroom 2 or more times during the night.
04
urge incontinence
Uncontrolled urine leakage after urgency
Judgment basis
01
History and Physical Exam
02
Patient Self-Completed Questionnaire
Patient self-administered questionnaires: such as Overactive Bladder Questionnaire (OAB-q), Overactive Bladder Score (OABSS), Urinary Incontinence Impact Questionnaire (II-Q), etc.;
03
3-7 day urination diary
04
Other
Urine analysis, urine culture, residual urine volume, bladder and kidney ultrasound, cystoscopy, CT, MR, urodynamics, etc.
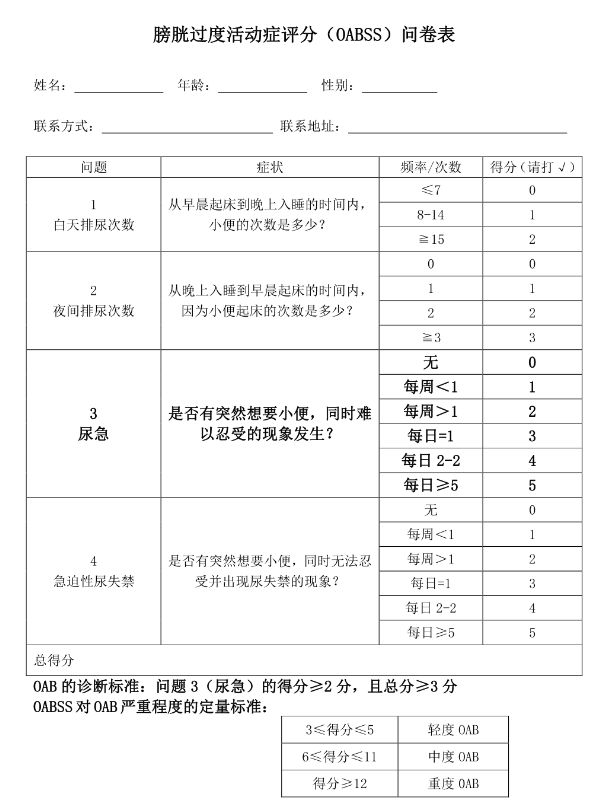
(OABSSS questionnaire)
Therapies
Treatment of overactive bladder can be divided into three categories: self-regulation, medication, and surgery.
01
Self-Regulation
1. Change bad lifestyle:
For example, pay attention to the intake of water and beverages, 6-8 glasses of water a day, avoid taking a large amount of water at one time, Do not drink more water near night ;

Adjust your diet to avoid foods and drinks that irritate the bladder, such as coffee, tea, chocolate, and certain medications;
Go to the toilet in advance, confirm the toilet in advance, make a toilet map, etc.
2. Bladder training:
Urine holding training: Don’t rush to the bathroom immediately when you have a urgency to urinate, hold it for a while, and wait for the feeling of urination to diminish.
Scheduled urination: Whether needed or not, buildinto the habit of urinating every hour, which can be gradually Increase the interval between urination until you can hold your urine for 3-4 hours.

Suppressing the urge to urinate: If you feel the urge to urinate before a fixed urination time, don’t stress, divert your attention, and take 5-10 slow, deep breaths. This connection can help Interfering with the brain’s “misinformation” of urgency.
3. Pelvic floor muscle training:
Imagine the action of stopping urination, sitting, standing or lying flat, try to contract the muscles for 3 seconds, then relax for 3 seconds, do it for 15-30 minutes, 150-200 times a day, can be divided into 2~ 3 times; 6-8 weeks as a course of treatment, 4-6 weeks for patients to improve, 3-month obvious effect.

02
Medication
Use antimuscarinic drugs or beta3-adrenergic agonists. Such as tolterodine, solifenacin, trospiron, mirabegron and other drugs. But use it under the guidance of a doctor.
03
Surgery
1. Bladder electrical stimulation
Inhibits unstable contractions of the detrusor muscle by electrical stimulation.
2. Other treatments
Such as intermittent catheterization, bladder enlargement, urinary diversion, etc.
————————————
References
Lightner DJ, Gomelsky A, Souter L, et al. Diagnosis and Treatment of Overactive Bladder (Non-Neurogenic) in Adults: AUA/SUFU Guideline Amendment 2019[J].J Urol.2019 Sep; 202(3): 558-563.
Corcos J, Przydacz M, Campeau L, et al. CUA guideline on adult overactive bladder[J]. Canadian Urological Association journal=Journal de l’Association des urologues du Canada 2017:142.
Sheng Guobin, Su Hang, Liu Changyan, et al. Treatment strategies for elderly patients with overactive bladder: 2017 Canadian guideline solutions
Editorial Team
Editor in charge: Dang Jiaying
Image source: Maker Post
Xiaoming Gong, MD
Former Associate Professor of Obstetrics and Gynecology, Peking Union Medical College Hospital
Former Deputy Director of Gynecology and Head of the Minimally Invasive Center of Shanghai First Maternity and Infant Health Hospital
Chief Specialist of Wo Medical Center for Minimally Invasive Treatment of Uterine Fibroids