
Introduction
Mycoplasma pneumoniae pneumonia is a common respiratory disease in children caused by infection with Mycoplasma pneumoniae, mostly in school-aged children. The survey shows that the incidence of Mycoplasma pneumoniae pneumonia in children is increasing year by year, accounting for 10% to 40% of children’s community-acquired pneumonia. Most of the children with early Mycoplasma pneumoniae pneumonia are often ignored, delaying the disease. Therefore, the rapid and accurate diagnosis of Mycoplasma pneumoniae pneumonia and the adoption of reasonable treatment plans are of great significance. This article will introduce these issues.
Diagnostics
The onset of Mycoplasma pneumoniae pneumonia in children varies in severity and severity, and may present with pulmonary manifestations such as fever, cough, and wheezing, and may also manifest with multi-system damage, such as muscle strength changes, headache, Nervous system symptoms such as unconsciousness and convulsions, digestive system symptoms such as nausea, vomiting, liver damage, joint and muscle pain, and various rashes. M. pneumoniae pneumonia may be difficult to diagnose based on clinical symptoms alone, and laboratory tests are required. In the early stages of infection, a positive PCR test may be accompanied by a negative serological test because it takes time for IgM antibodies to develop. During the recovery period, a positive serology test may be accompanied by a negative PCR test. Therefore, there is currently no single method that can accurately diagnose M. pneumoniae infection. For suspected patients, PCR and IgM combined detection is ideal for early diagnosis, especially in children.
Acute mycoplasma infection is diagnosed in patients with suspected clinical features and one of the following 3 laboratory findings:
①Seroconversion (specific Mycoplasma pneumoniae IgM changed from negative to positive);
②Increase in specific antibodies within two weeks (2-fold increase in Mycoplasma pneumoniae IgM/4-fold increase in specific IgG by titer or dilution test);
③The PCR result was positive.
Although M. pneumoniae infection is self-limiting, persistent fever and/or more severe extrapulmonary manifestations may also occur when treatment is delayed or with ineffective antibiotics. Therefore, early diagnosis and treatment can help prevent deterioration. The first-line drugs for the treatment of Mycoplasma pneumoniae infection are macrolides, the second-line drugs are tetracyclines and fluoroquinolones, and other drugs are glucocorticoids and immunoglobulins.
Treatment process
The correct choice of antibiotics is the key to the treatment of Mycoplasma pneumoniae pneumonia in children. The specific treatment process can be referred to the following figure.
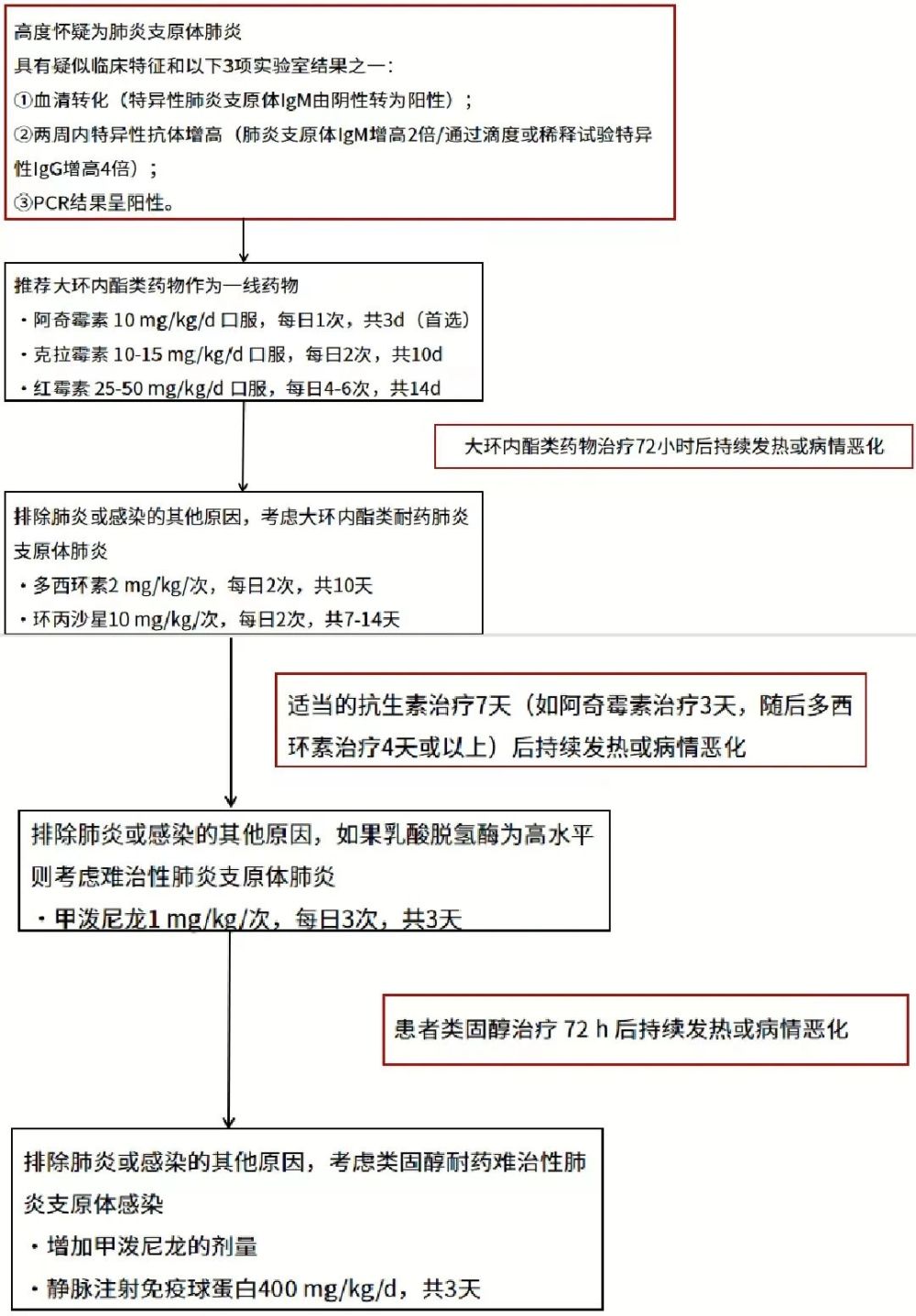
Figure 1 Treatment flow of Mycoplasma pneumoniae pneumonia in children
References:
1. Wang Lin. Research progress on diagnosis and treatment of Mycoplasma pneumoniae pneumonia in children[J]. Journal of Shangluo University, 2022,36(04):30-35.
2. Tsai TA, Tsai CK, Kuo KC, Yu HR. Rational stepwise approach for Mycoplasma pneumoniae pneumonia in children. J Microbiol Immunol Infect. 2021 Aug;54(4):557-565 .
3. Feng Bihong, Dai Kona, Yang Haohao, Mi Kezhe, Shi Hongbo. Analysis of clinical characteristics of Mycoplasma pneumoniae pneumonia in children [J]. Zhejiang Medicine, 2019,41(11):1194 -1196+1200.
4. Ming Dan. Advances in drug treatment of children with Mycoplasma pneumoniae pneumonia[J]. Clinical Medicine, 2021,41(01):120-122.