This is a case from many years ago. I want to share it with you. I hope everyone can learn from it.
Case introduction:
The patient is a 40-year-old male. Subtotal gastrectomy and gastroduodenal anastomosis were performed under continuous epidural anesthesia due to gastric ulcer perforation. (Note: At that time, it was still in the era of anesthesia where “one needle goes all over the world”.)
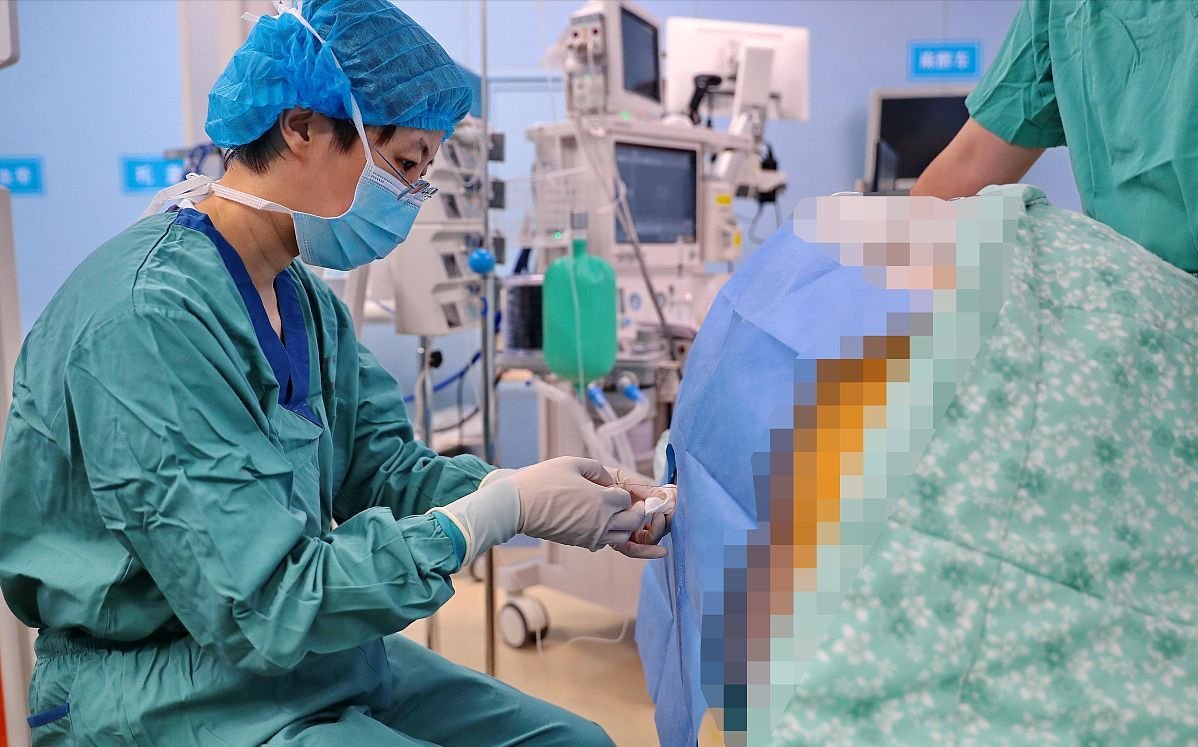
< span>Everything is ready, the anesthesiologist performs a puncture through the T8-9 intervertebral space. However, the puncture encountered difficulties. After more than ten minutes of effort, the puncture needle was still unable to penetrate the target. As a result, the anesthesiologist changed the epidural puncture to the lateral approach, and finally succeeded.
The textbook clearly states that the lateral entry method is suitable for elderly patients with severe calcification or difficult puncture. Therefore, there is not much problem in choosing side entry puncture here.
After water injection and air injection without resistance, the placement of the epidural catheter was smooth. A few minutes after the experimental amount of local anesthetic was injected through the catheter, 10 ml of local anesthetic was added after no abnormal performance.
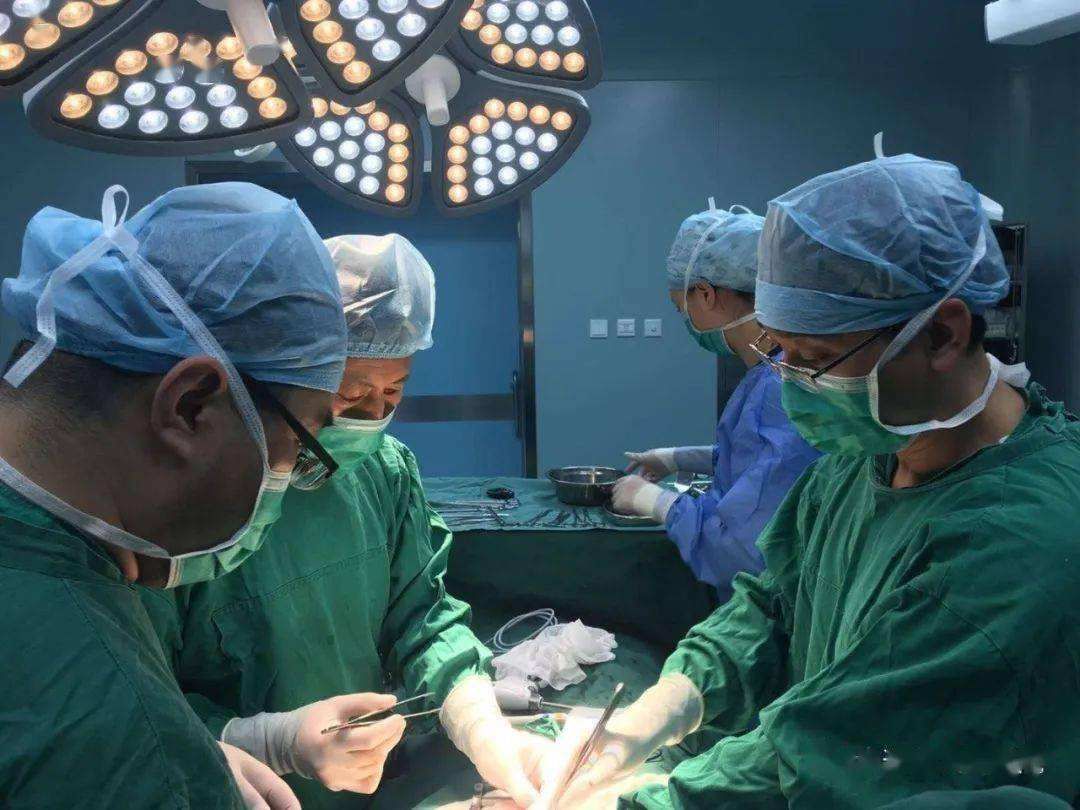
Once the results are good, the surgery begins. The operation lasted 3 hours, and 6 hours after returning to the ward, the patient felt soreness, numbness, twitching, and restlessness in both lower extremities.
At that time, sedation was given because of the patient’s physical movement due to discomfort.
Several hours later, bilateral sub-groin pain disappeared, abdominal wall reflexes, cremasteric reflexes, and knee tendon reflexes disappeared, and Babinski’s sign was negative.
After 16 hours, the sensation below the T8 plane disappeared, and both lower limbs were paralyzed. Plain CT scan of the spinal cord showed gas density images in the spinal cord at T6-9 levels, with clear boundaries, located in the center of the spinal cord, most prominent in the thoracic 7 plane, annular high-density areas in the subarachnoid space, and inhomogeneous structures in the dural sac.
At this point, it was confirmed that spinal cord injury caused by epidural puncture.
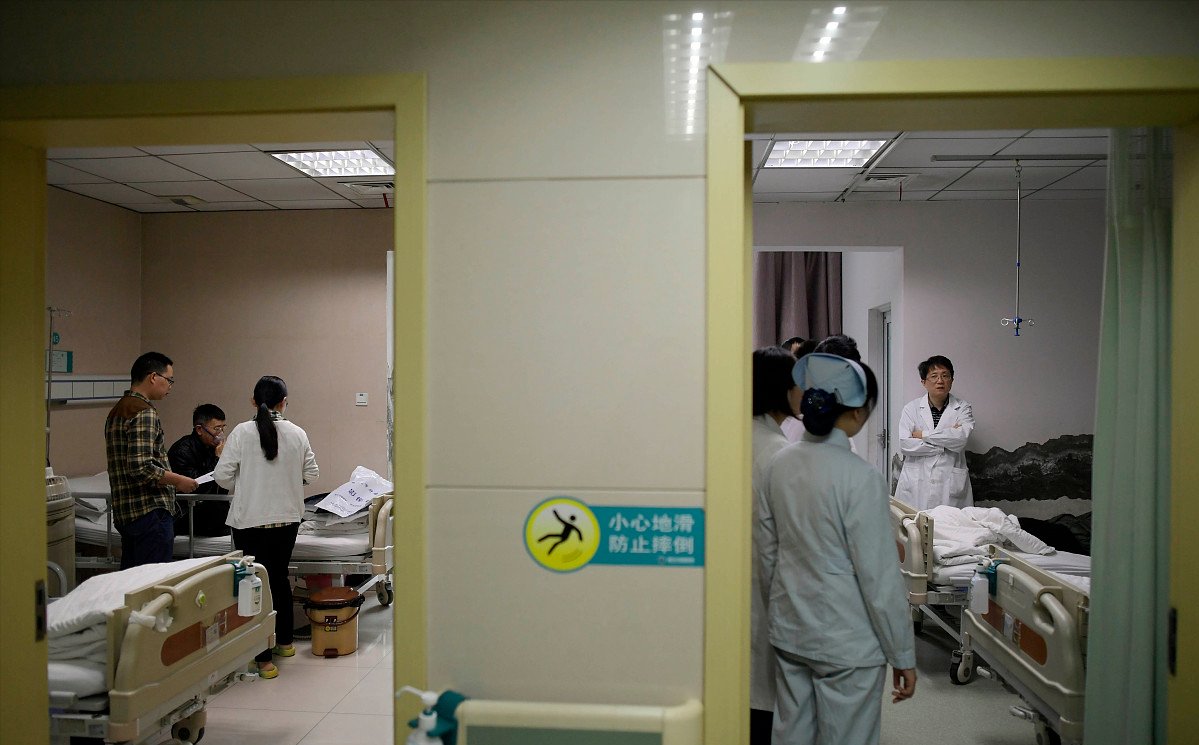
However, because the hospital was worried about family members being held accountable at that time, no active medical measures were taken. Five months later, CT re-examination showed that the gas accumulation and bleeding were completely absorbed, but the paralysis symptoms did not improve, and it was confirmed that he was paralyzed for life.
Anyone who is responsible for the problem, what are the lessons learned from this case?
First of all, high-level spinal canal puncture must be performed by a senior anesthesiologist. Senior anesthesiologists with years of puncture experience can improve the success rate of spinal canal puncture and detect abnormalities in time. Like this case of anesthesia, an experienced anesthesiologist may find that the puncture needle has reached the target through the layered feel of the puncture, instead of repeatedly puncturing, injecting air and water, and “searching for negative pressure”.
Secondly, the purpose of the epidural test volume needs to be very clear. The amount of epidural experiments was mainly found to have mistakenly entered the blood vessels and the subarachnoid space. Second, it is found that the catheter is mistakenly inserted into the subdural space, one side of the spinal nerve root, or intraspinal injection. Here, focus on intraspinal injection: Intraspinal injection, patients generally have severe pain. Even, the patient may make an “ah” sound due to pain. At this time, we should not blindly reprimand the patient “don’t move”, but promptly ask if there is any abnormality.
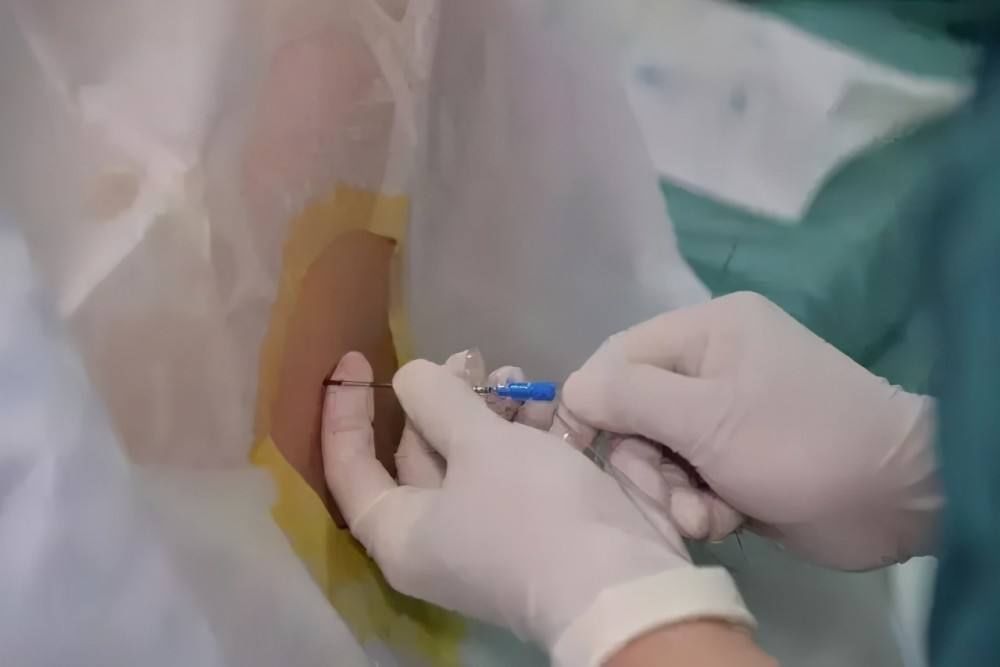
Again, we emphasize a detail: when puncturing, especially the high epidural For puncture, be sure to find an assistant to control the patient’s body movements. In such a state of high tension, there must be some patients who cannot control their physical movements. Once there is physical movement, it may affect the feel or judgment during the puncture process and lead to complications. At the same time, I also say to the patient: I know you are nervous, but you should try your best to control your body, and you must cooperate with the doctor’s operation.
Finally, we recommend: in the process of high epidural puncture, once encountering difficulty in puncturing, either give up in time, or choose puncture under ultrasound visualization. In this important position, neither our doctors nor our patients can afford it!
【Warm reminder】Please pay attention, here are a lot of professional medical science, to reveal the secrets of surgical anesthesia for you~