According to WHO’s latest “Cumulative Cancer Risks Before Age 75 in Various Countries”, the probability of Chinese people getting cancer before age 75 is 20.6%, which is equivalent to that for every 5 Chinese people, 1 in 1 will develop cancer before age 75. In recent years, there are more and more cancer patients in China, but the cancer mortality rate is decreasing. Radiation therapy, as one of the main means of treating malignant tumors, plays an important role in improving the cure rate of cancer. However, many people’s understanding of radiotherapy is still at the stage of “big side effects”, and radiotherapy has also been dyed with a nervous color. Fear stems from the unknown, let us uncover the mystery of radiotherapy and explore the “true face” of radiotherapy.
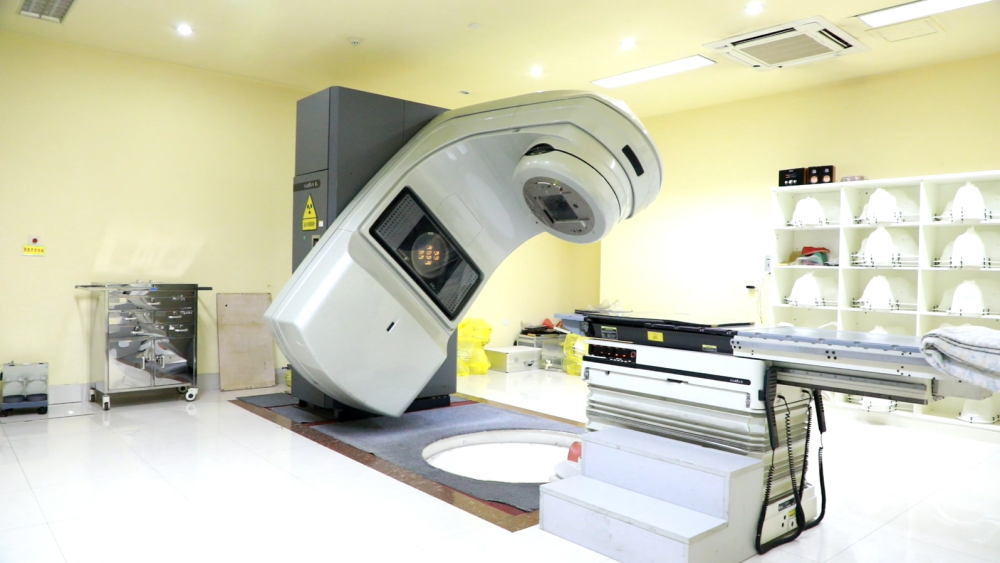
Radiation therapy is a local treatment method that uses radiation of different energies to irradiate the tumor to inhibit and kill malignant tumor cells. It can be used alone or in combination with surgery, chemotherapy, etc. comprehensive treatment. Before radiotherapy, physicians will discuss and formulate the most appropriate individualized radiotherapy plan based on the detailed medical history, signs, pathology, laboratory and imaging examination data of each patient. Let us take the radiation therapy of head and neck tumors as an example to introduce the process of radiation therapy.
First, body membrane production
After the radiotherapy plan is determined, doctors, physicists and technicians will select and formulate a fixed mold according to the specific conditions of the patient to ensure good position repeatability during each radiotherapy, and try to make the patient feel comfortable. Reduce the impact of body position change error on precise radiotherapy and ensure accurate radiotherapy. At present, the commonly used body membranes in the head and neck radiotherapy department of Shandong Otolaryngology Hospital are: head mask, neck and shoulder membrane, head, neck and shoulder membrane, and phantom.
Second, simulated positioning
In order to obtain accurate radiotherapy results, the physician positions the patient on the flat CT bed according to the position of the body membrane when making the body membrane. The corresponding parts are scanned by CT, and after the scanning, the images will be directly transmitted to the treatment planning workstation through the network.
Three, target area delineation
For radiotherapy, the core technology is to delineate the target volume, that is, to determine the range of radiotherapy. The physicist imports the image into the planning system for preliminary processing to ensure the high quality of the image. According to the size and shape of the tumor, the diagnosis and treatment doctor outlines the target area and the important organs that need to be protected on the corresponding CT levels. Because cancer cells may metastasize, which brings great challenges to the delineation of the target area, radiotherapy physicians need to have solid oncology knowledge and rich clinical experience to determine the area where the tumor may metastasize, and use an appropriate dose of a And radiation, while also protecting major organs from radiation damage.
IV. Plan Evaluation
After determining the range of radiotherapy, the physicist uses different algorithms to generate the optimal radiotherapy plan according to the doctor’s target area and prescribed dose requirements, so that the radiation dose is highly concentrated in the target area and the surrounding area is normal. The exposure to vital organs is controlled within the dose limit. In addition, in the design of radiotherapy plans, close communication with doctors is required, and complex target volume plans may have to be revised and weighed repeatedly. After the plan design is completed, the radiation therapist will conduct a confirmation review of the plan.
V. Radiotherapy Plan Verification and Treatment
Theoretical treatment plan needs to be verified under actual conditions, and the radiotherapy center location verification, field verification and dose verification should be carried out before the plan is carried out. Dose verification is to verify whether the radiation dose received in the body is consistent with the radiation dose designed by the planning system through the human body simulation phantom. Multiple trials ensure the accuracy of the treatment site and the safety of other organs. After the verification is passed, the patient can lie flat on the treatment couch, keep the same position as the positioning, and enter the treatment process.
Professional radiotherapy doctors can control the site of radiotherapy very precisely, without affecting other organs, and patients can relax their minds to receive radiotherapy. However, the level of professional medical technology is important, and the patient’s emotions also play a key role in the anti-cancer process. Cancer patients should correctly understand “cancer” and its treatment methods, avoid blind fear, and accept treatment with a positive and optimistic attitude.