Text/Picture Yangcheng Evening News All Media Reporter Zhang Hua
On September 15, the “National Science Popularization Day” kicked off and will last for a week. In order to popularize the knowledge of cervical cancer prevention and treatment to the public, the “Cervical Cancer Prevention and HPV Vaccine Awareness Survey Results” (hereinafter referred to as “Research Results”), guided by the China Maternal and Child Health Association and supported by GlaxoSmithKline China, was published online on September 19. Officially released. It is reported that the survey is from 4,393 female respondents aged 16-45, aiming to understand the types and infection routes of HPV (human papillomavirus), the prevention methods of cervical cancer, and the HPV vaccination behavior and willingness of women of the right age. etc. cognition.

Yu Xiaoqian, Executive Vice President and Secretary General of China Maternal and Child Health Association
At the meeting, Yu Xiaoqian, executive vice president and secretary general of the China Maternal and Child Health Association, said: “Cervical cancer is a common gynecological malignancy in women, and it is currently the only cancer that can be prevented by vaccination. It is hoped that the release of the “Cervical Cancer Prevention and HPV Vaccine Awareness Survey Results” can help women of appropriate age to master the scientific knowledge of cervical cancer prevention!”
More than half don’t know about high-risk HPV types: HPV 16 and 18 are the “culprits”
The “Survey Results” showed that the interviewed women lacked knowledge about HPV virus and HPV vaccine; Only 30% of them understand and act; in addition, the women interviewed are very willing to vaccinate themselves with HPV vaccine and bring their daughters to vaccinate, but due to subjective factors such as valence, safety and supply constraints, there are many waiting for vaccines, and women of appropriate age Mobility needs to be improved urgently.
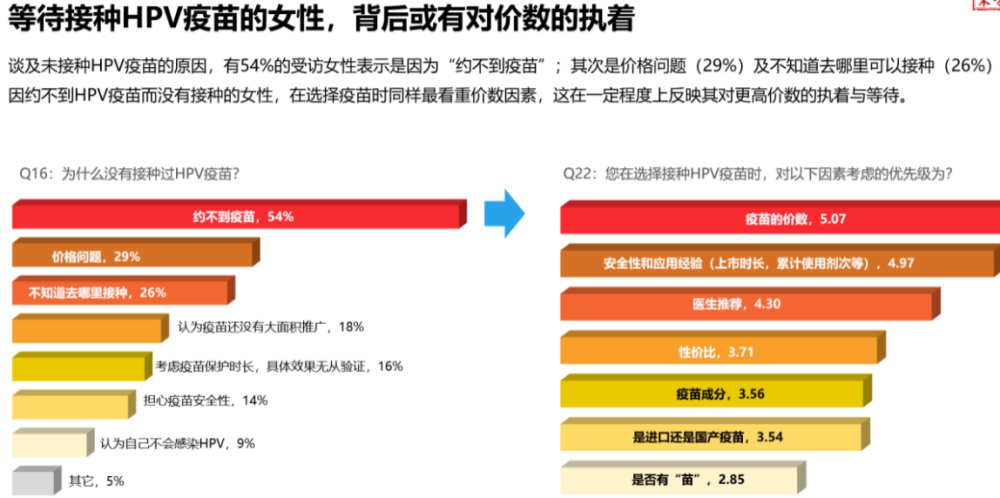
“Research Results” shows that “no vaccine appointment” is actually the result of pursuing high-priced vaccines
The main data of the “Survey Results” showed that the women interviewed had a high degree of awareness of HPV, but they did not know much about the virus type and its risk. At the same time, the current HPV vaccination rate in China is still relatively low. Although the women interviewed and their daughters are highly willing to be vaccinated, they are affected by subjective factors such as valence, safety, and objective vaccine accessibility. Lack of motivation.

Zhao Yun, Deputy Chief Physician, Department of Gynecology, Peking University People’s Hospital
It is worth noting that the “Survey Results” also showed that 95% of the interviewed women had heard of HPV (human papillomavirus), and 55% of the interviewed women could not accurately identify the common high-risk type. In this regard, Zhao Yun, deputy chief physician of the Department of Gynecology of Peking University People’s Hospital, explained: “There are more than 200 HPV types that have been identified. According to the difference in carcinogenicity, HPV is divided into high-risk and low-risk types. High-risk HPV types It is the ‘culprit’ that causes cervical cancer. There are 14 known high-risk HPV types, and HPV16 and 18 are the most important high-risk types, causing about 84.5% of cervical squamous cell carcinomas in China. In China, female High-risk HPV infection presents two peaks, the first peak age is 15-24 years old; the second peak infection age is over 40 years old. Before the peak period of infection, vaccinate HPV as soon as possible. In addition, vaccinate HPV vaccine It is not ‘everything is good’, and regular cervical cancer screening is still required, and HPV vaccination + cervical cancer screening is the perfect combination to prevent cervical cancer.”
Over 80% will be vaccinated, but only 30% will be vaccinated
Obsession with high valence and waiting may be an important reason for low vaccination rates
HPV vaccination as a primary preventive measure is the most important line of defense against cervical cancer. From a global perspective, women aged 9-45 in my country have more choices, and there are 5 types of HPV vaccines to choose from, including imported bivalent, quadrivalent, nine-valent, and 2 domestic bivalents. According to the survey results, only 30% of the women surveyed had received the HPV vaccine. Regarding the reason for not getting the HPV vaccine, 54% of the interviewed women said that it was because “the vaccine was not available”. Among the women who did not get the HPV vaccine and did not receive the vaccine, the number of waiting for the high price ranked first.
There are a large number of school-age women in my country. Under the limitation of accessibility under objective conditions, although the overall willingness to be vaccinated is high, the actual vaccination rate is not high. The “Research Results” also reflects the persistence and waiting for high prices behind this. In this regard, Wang Linhong, honorary chairman of the Women’s Health Branch of the Chinese Preventive Medicine Association, suggested: “Don’t wait blindly. Women can choose flexibly according to vaccine resources and their own economic conditions. The earlier the HPV vaccine, the better! In China, 84.5% of cervical cancers are It is caused by persistent infection of HPV types 16 and 18. The currently available HPV vaccines cover these two types and can prevent most cervical cancers and precancerous lesions. The bivalent HPV vaccine is very good. preventive effect.”
In addition, the protective power of vaccines, which everyone is concerned about, is actually related to the components of vaccines. In addition to antigens, adjuvants are also important components. The adjuvant used in each HPV vaccine is different, and vaccines with innovative adjuvants will stimulate a higher immune response in the body and provide stronger and longer-lasting protection. However, both clinical trials and real-world studies have confirmed that HPV vaccines with innovative adjuvants are effective against other types of vaccines.Oncogenic HPV also has a good cross-protective effect.
As to whether the HPV vaccine needs to be “replaced” or “strengthened”, Professor Wang Linhong emphasized that the mathematical model of clinical data predicts the long-term protective effect of HPV vaccine, and the protection time can be long up to 50 years. In addition, authoritative organizations such as the World Health Organization and the American Advisory Committee on Vaccine and Immunization Practice (ACIP) have recommended that after completing the whole course of vaccination with one HPV vaccine, it is not recommended to boost the HPV vaccine. In the current situation of tight supply of HPV vaccine, early vaccination is more important than high price, and being infected while waiting will not be worth the gain.
The best time to get the HPV vaccine: 9-14 years old first, then now
Regardless of whether they have daughters or not, about 92% of women surveyed expressed their willingness to be actively vaccinated. Even so, 61% of the women surveyed had insufficient awareness of the optimal age for vaccination between the ages of 9-14. Among women who were unwilling or unsure about taking their daughters for HPV vaccination, 29% believed that their daughters would not be infected with HPV if they were asexual or had no unsafe sex.
Professor Zhao Yun further explained that sexual behavior is an important risk factor for HPV infection. As a preventive vaccine, the best preventive effect can be obtained by vaccinating women who have not had sex with HPV vaccine. For girls who are at the best age for vaccination, parents should pay attention to the timing of vaccination. The earlier the younger the better, the better the benefit. The application of HPV vaccine in my country is for women aged 9-45. Even if women who miss the optimal vaccination age of 9-14 years old, sexually active and adult women can still benefit from HPV vaccination. The second best vaccination age That is the present moment. In addition, all the HPV vaccines currently on the market cannot cover all high-risk HPV types, that is, the protection rate is not 100%. After the HPV vaccine is vaccinated, regular screening should be paid attention to, and the two-pronged approach can better prevent cervical cancer.
Source | Yangcheng Evening News·Yangcheng Pie
Editor | Lin Qingqing