5-year-old Tiantian is ignorant, but she knows that her mother will carry that pink leather bag with her wherever she goes, because it is the battery of her mother’s “heart”.
2017 was a year of ups and downs for 29-year-old Cui Liao. She gave birth to the lovely sweet that year, and a few months later was diagnosed with dilated cardiomyopathy, which can cause heart failure, arrhythmias and sudden death.
Liao Cui did not escape heart failure, and her condition later progressed to a refractory end-stage. According to the research results of Academician Gao Runlin and Professor Wang Zengwu of Fuwai Hospital in 2019, about 13.7 million people aged 35 and above in my country suffer from heart failure.
For patients with end-stage heart failure, there are generally three options: heart transplantation, palliative care, and implantation of a ventricular assist device. Liao Cui chose the last one.
On August 30, 2019, she underwent artificial heart implantation at Wuhan Union Hospital. After surgery, a 180-gram, 50-millimeter-diameter blood pump was added to the apex of her left ventricle. The impeller, at more than 2,000 revolutions per minute, helped her left ventricle carry blood into the aorta.
She put the battery and external controller in a pink leather bag and carried it with her at all times.
At the time of the occasional healing interview, Liu Cui had been with her artificial heart for over 900 days.
In her opinion, nothing is more important than living a good life. Just like the morning of the operation, facing the unknown, she wrote in the circle of friends: “I have prepared for the worst, but I still hold the greatest hope, praying for a smooth operation and a safe discharge from the hospital… Goodbye, goodbye by fate! “

Liao Cui with a pink leather bag crossbody
Image source: provided by Liao Cui
Artificial heart is the final choice
February 23, 2017 was the day before Tiantian was born. Liao Cui, accompanied by her family, went to the hospital for fetal heart rate monitoring. She told the doctor that she was very tired and hoped to have an early caesarean section.
The doctor performed a color ultrasound on her heart, and when she saw the results, she quickly transferred her to a tertiary hospital.
In a tertiary hospital in Wuhan, after reading Liao Cui’s electrocardiogram, the doctor pushed him into a wheelchair and said that the situation is very serious, and there is a possibility of one corpse and two lives.
Actually, Liao Cui had feelings during pregnancy. Her electrocardiogram showed abnormality many times during the prenatal check-up. When she took a bath, she just touched her stomach and saw the rapid rise and fall of her chest; she was pregnant. At week 37, the doctor suggested that she climb stairs to exercise, but she couldn’t even climb one floor.
The explanation she got from the doctor for these cases was that it was a sign of increased heart burden after pregnancy and nothing to worry about, so she didn’t take it to heart.
After the birth of her daughter, Liao Cui was sent to the Cardiology Department. She remembered that the doctor judged that her condition was perinatal cardiomyopathy, and the heart would recover within six months after the burden was relieved. A month later, another tertiary hospital gave the same diagnosis.
But Liao Cui’s health did not improve with the end of the perinatal period. She was so weak that she couldn’t even get up or take a shower, and she didn’t stop vomiting. These are all symptoms of heart failure.
Li Qianzhen, Deputy Chief Physician of Cardiac Surgery, Union Hospital Affiliated to Fujian Medical University, told Occasionally cured patients with severe heart failure or at the end-stage, due to reduced cardiac ejection, other organs will be affected , venous congestion, tissue ischemia, such as gastrointestinal congestion can cause vomiting. Some patients with end-stage heart failure also have difficulty breathing and lower extremities edema.
Liu Cui has no breathing problems, but suffers from daily vomiting. In early June 2017, she was diagnosed with dilated cardiomyopathy and end-stage heart failure by Wuhan Union Medical College Hospital and needed to be prepared for heart transplantation.
China Heart Failure Diagnosis and Treatment Guidelines 2018 shows that heart transplantation is an effective treatment for end-stage heart failure. Between 2015 and 2019, 2,262 heart transplants were performed and reported in China, and the one-year survival rate of patients was 85.2%.
Not every patient will be able to receive a transplant. Li Qianzhen introduced that in the early days, many patients could not wait for a suitable heart donor. The premise of transplantation was that someone donated and the matching was successful. Some patients died before they waited for the person. His department sees about 80 patients with end-stage heart failure a year, and less than half of them end up receiving transplants.
Liao Cui was a little afraid of heart transplantation. She knew that the operation was expensive, and she was worried that she would not survive the first year after the operation. In the following two years, she went to many hospitals in China for treatment. It was only after a few days of rescue that she woke up. Liao Cui made up her mind to accept the transplant.
In 2019, Liao Cui was hospitalized in a hospital in Beijing. On the pillow was “No Limits in Life” given by a girl in the same ward. The author Nick Hu Zhe was born without limbs. (Source: Provided by Liao Cui)
On June 17, 2019, Liao Cui was admitted to Wuhan Union Medical College Hospital, and 9 days later joined the COTRS system (China Human Organ Distribution and Sharing Computer System) transplant appointment list. At 1.68 meters tall, she weighed only 40 kg and had a left ventricular ejection fraction (LVEF) of only 16%, while the normal LVEF for a healthy adult is 55% to 65%.
Even if the family is mentally and financially prepared, the body may not be eligible. A certain antibody in Liao Cui’s body is too high, and the rejection reaction after transplantation will be very serious. The doctor told her that she would either not be able to get off the operating table, or she would experience rejection after the operation.
To survive, Liao Cui has only one last way: implanting a left ventricular assist device, that is, installing an artificial heart.
Add a “motor” to the heart
Liao Cui once read from the news that in October 2018, Wuhan Union Medical College Hospital successfully completed the first artificial heart implantation operation in Hubei Province.
Later in the doctor’s office, Liao Cui saw a mannequin with a left ventricular assist device (LVAD). She found that the artificial heart was not what she imagined.
Liao Cui originally thought that the artificial heart was to take out the original heart and install a mechanical heart. Her vision shares similarities with the Total Artificial Heart (TAH). At present, there are three types of TAH that have entered the clinical application stage in the world. Due to the high price and irreversibility, its application still faces many problems.
Li Qianzhen, Deputy Chief Physician of Cardiac Surgery, Union Hospital Affiliated to Fujian Medical University, also believes that TAH is not yet mature enough.
With an LVAD implanted, the patient’s own heart is still there, except for an extra golf ball-sized pump at the apex of the left ventricle. After the blood in the left ventricle flows into the pump from the inlet tube, the pump will rotate at a high speed under the action of the external controller to push the blood through the artificial blood vessel into the aorta, thereby maintaining the blood circulation.
Li Qianzhen likened the artificial heart to a new car engine, “The heart is your original engine. After this engine is weak, we will install a new engine for you, which will replace or Help the original engine work, and your heart can rest.”
June 2019, Liao Cui was hospitalized while awaiting surgery. What will be implanted in her body is a new generation of fully magnetically levitated artificial heart VAD developed by a medical technology company in Suzhou. The pump has a diameter of 50 mm, a thickness of 26 mm and a weight of about 180 grams.
From the classification of the development of artificial heart technology in the Intermacs Annual Report of the United States, VADs are generally divided into two generations: pulsatile VADs and rotary VADs.
The old generation is a pulsatile VAD. Take the Novacor produced by World Heart Company in the United States as an example. It can simulate the action of the heart and pump blood to the aorta through the contraction and relaxation of the airbag in the device. , but its shortcomings are obvious: the volume is too large and can only be implanted in the abdominal cavity; the balloon and mechanical moving parts are easily damaged; it is easy to form thrombus around the valve. Overall, the clinical outcomes of pulsatile VAD are suboptimal.
Based on the concept of making the VAD better complete the blood pumping function, a new generation of rotary VADs appeared. According to different technologies, the international medical community classified them as sliding (contact) bearing , Hydrodynamic suspension, full magnetic suspension. Among them, the fully magnetic levitation artificial heart is exquisite and small, and the damage to the blood is lower, and it has become the mainstream artificial heart product in the world.
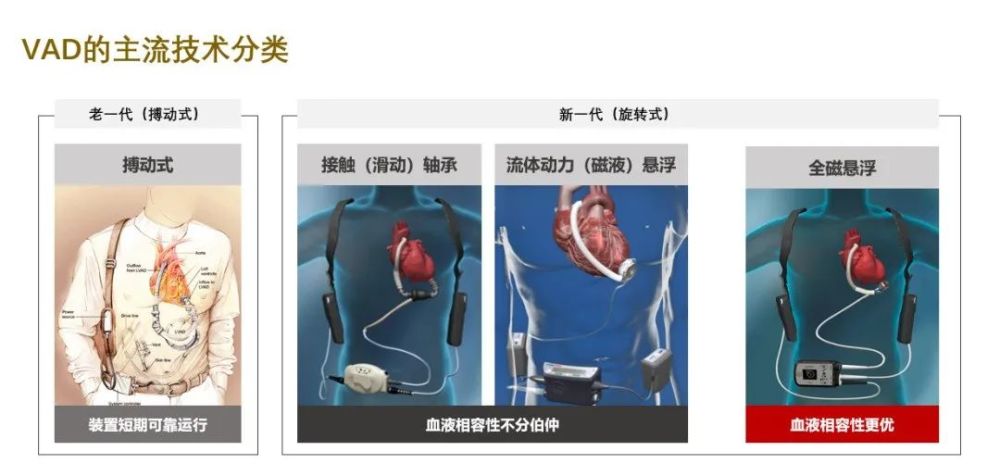
Classification of VAD
Image source: provided by Liao Cui
Therefore, for Liao Cui, the implantation of the full magnetic levitation artificial heart is less invasive, and the probability of postoperative gastrointestinal bleeding, stroke, infection and other adverse events is also lower.
A near-normal life with an artificial heart
While waiting for the operation, Liao Cui and her husband often did handicrafts, painting, and diamond painting in the ward, and also volunteered to help the children in the same ward with English lessons.

While waiting for the surgery, Liao Cui and her husband finished painting all the paintings in a hand-painted book (Source: provided by Liao Cui)
Liao Cui is looking forward to returning to a normal life after being discharged from the hospital. She made a list of “must eat after surgery”. Favorite food. But in fact, her vomiting did not stop until the 4th month after being discharged from the hospital, after which she followed the list and fulfilled her wishes one by one.
The surgery was scheduled for August 30, 2019. Liao Cui was afraid that she would not be able to wake up again, so she told her husband all her password information, and sent a message to her friends to say goodbye, saying “Goodbye by fate”.
On the morning of the surgery, Liao Cui wrote “Goodbye by fate” in the circle of friends (Photo: Courtesy of Liao Cui)
Fortunately, the operation was successful and Liao Cui was transferred from the ICU to the general ward a week later. She noticed a different part of her chest, as if there was something more, where the CH-VAD’s impeller was assisting her heart at over 2000 RPM.
After surgery, a white cable was threaded through Liao Cui’s lower abdomen. One end of the cable was connected to the blood pump in the body, and the other end was connected to the external controller. The part that remained outside the body was about 60 It is centimeters long and the thickness is similar to that of a mobile phone charging cable. In order to prevent infection, she disinfects and changes the dressing for the part where the cable passes through every day.
The external controller is also connected to 2 batteries by wires, when one is working, the other is not used as a backup. Each implanter receives 6 batteries from the manufacturer, each of which lasts about 8 hours. Liao Cui keeps a battery in her car, and every time she goes out, she checks the battery to make sure it is full.
The total weight of the controller and 2 batteries is about 1.4 kg, which is similar to carrying 3 bottles of 500 ml mineral water with me. Liao Cui often feels that her shoulder hurts when she is straddling them.
In September 2019, Liu Yiming (pseudonym), who suffered from the same condition as Liao Cui, also had an artificial heart implanted. When the air entered the lungs unobstructed and was exhaled unimpeded, he found that I don’t have to pant heavily, and I don’t have the feeling of suffocation before.
Currently, Liu Yiming’s sleep and drinking water cannot fully return to the state before the illness, but he is content. When he goes out, he is used to carrying 2 batteries in addition to the 2 batteries necessary for the device. After getting to know Liao Cui, Liu Yiming told her to wear a vest with multiple pockets when going out, and put the batteries in the pockets on both sides to reduce the burden on her shoulders.

Artificial Heart Battery
Image source: provided by Liao Cui
Because the controller and battery can be damaged when exposed to water, put them in the shower bag and put a waterproof tape over the body when the patient bathes. At the same time, they can no longer go swimming, hot springs, and water-related activities.
In addition, to avoid exposure to high magnetic fields, they need to stay away from security checks and induction cookers as much as possible.
With an artificial heart implanted, patients cannot fully return to their previous lives. Liu Yiming had been a high school teacher for more than ten years. He wanted to return to his post after the operation, but the school was worried about his health and arranged for him to organize materials and help new teachers with research. He couldn’t help feeling a little disappointed.
Later, due to the heat in the office and prolonged sitting, Liu Yiming’s abdominal wound showed signs of festering. After thinking about it again and again, he asked the school for sick leave to devote more energy to his talk show.
Few people continue to work or find new jobs after an artificial heart is implanted. Most of the 18-member group of artificial heart implanters set up by Cui Liao are unemployed. Liao Cui believes that by empathy, employers will be apprehensive because they are worried about accidents.
In addition, after the artificial heart is implanted, some implanters also face difficulties in psychological acceptance, such as having a “sense of incompleteness” and thinking that there is something in their body that does not belong to them. Liu Yiming felt that when he was walking on the road, it seemed that someone was looking at him. Sometimes, after explaining to the subway staff why they couldn’t check in, their eyes would make him uncomfortable.
Liu Yiming doesn’t want to be seen as an “abnormal person” or “patient”, but only wants to be an ordinary person. When performing a talk show, he hides cables, controllers and batteries to keep the audience from getting nervous and to keep himself from “feeling weird”.
Mechanisms need to be established to improve the quality of life of implanters
Liao Cui and Liu Yiming are lucky to some extent, because not every patient with end-stage heart failure can be implanted with an artificial heart.
Last year Li Qianzhen met a patient who missed the opportunity for implantation and eventually passed away. Li Qianzhen once suggested that he implant an artificial heart immediately, but considering the cost, he hesitated for two weeks before agreeing. At that time, his condition deteriorated and his body could no longer bear the implantation operation. Whenever he thinks of this patient, Li Qianzhen feels very sorry.
According to the introduction of the research and development company, the artificial heart has three functions: as an adjuvant therapy (BTR) before the recovery of cardiac function, it provides short-term support for the patient, and it can be removed after the recovery of the cardiac function; Bridging treatment (BTT) before heart transplantation, to buy more time for patients to wait for the heart source; as long-term treatment (DT), to provide patients with permanent replacement.
A patient from Hubei known to Liao Cui and Liu Yiming underwent artificial heart removal surgery in July 2021. Liu Yiming envied him very much: “I can’t wait to take it out and replace it with myself, but I still have to work hard on my own.”
But Liu Yiming knew that he had little hope of getting off the plane. During the re-examination, the doctor told him that, as an old patient for more than ten years, his heart muscle fibers have been partially calcified due to long-term rupture, and it is difficult to recover even with the assistance of an artificial heart.
Two and a half years after the implantation, Liao Cui also learned from the doctor that her heart function has not changed compared with before, “As long as it does not deteriorate, it is good news for you. Don’t expect it to get better.”
This means that Liao Cui and Liu Yiming may need to live with artificial hearts for life.
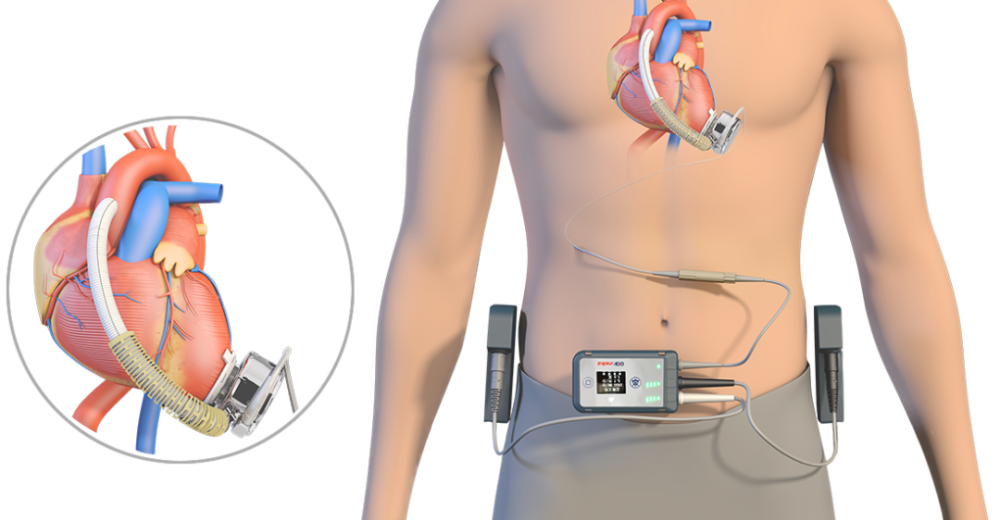
Schematic of Cifu VAD
Image source: official website of a medical technology company in Suzhou
In fact, long-term treatment is the most mainstream use case for artificial hearts today, with more than 50% of implants worldwide.
In this context, how to provide implanters with a higher quality of life has become one of the key concerns of VAD developers.
Relevant personnel of this medical technology company in Suzhou, which developed VAD, told Occasional Cure that the efficacy of VAD not only depends on the performance of the device, but also greatly depends on the choice of treatment timing and the postoperative recovery of patients. long-term management.
Therefore, on the one hand, it is necessary to establish a heart failure management network for each region to improve the quality of patient selection; on the other hand, in order to improve the long-term treatment effect, it is necessary to After home, provide them with technical support on VAD use at any time until the end of use.
In patient selection, the assessment of the implant should be comprehensive, including medical, social, psychological, physical, and cognitive assessments.
Patients must also undergo a complete and adequate preoperative examination prior to implantation surgery. Because for very sick patients, if they choose implantation without adequate examination, their long-term quality of life may not be guaranteed, and there is also the risk of perioperative infection and multiple organ failure.
Under ideal conditions, multidisciplinary experts such as cardiology, cardiac surgery, nursing team, and intensive care team should participate in the diagnosis and treatment of artificial heart implanters, that is, the multidisciplinary diagnosis and treatment model (MDT) should be adopted. .
In addition, long-term management of patients after surgery is also required for implanters to have a higher quality of life.
After the artificial heart is implanted, the patient must develop new habits: Change the dressing every day, take anticoagulant drugs, try to avoid the equipment touching water, and keep away from the high magnetic field environment. Adjust past exercise patterns. These all place certain requirements on patient compliance, but not everyone can strictly follow the doctor’s orders all the time.
At the same time, the implanter may encounter various problems, such as creating a “sense of incompleteness”, and what to do with the controller’s highest level of alarm.
For these two reasons, it is necessary to build a multi-party VAD post-operative management system. Li Qianzhen mentioned that some hospitals will carry out psychological intervention for implanters. He hopes that in the future, personnel with professional backgrounds can follow up patients regularly and provide psychological support.
In June 2021, the Centers for Medicare and Medicaid Services (CMS) released the National Health Care Coverage Indicators (NCDs) for VAD, setting the Staffing – In addition to at least 1 physician with experience in cardiothoracic surgery, 1 cardiologist with advanced heart failure training, 1 VAD program coordinator, 1 social worker, 1 palliative therapist.
According to the Suzhou-based medical technology company, in Europe and the United States, the full-cycle treatment management of implanters is usually included in the hospital’s VAD program. In this project, doctors, coordinators, rehabilitation specialists and other social workers and manufacturers will jointly provide help and services for implanters. Among them, the coordinator generally has a nursing background and is a registered nurse. When the implanter encounters difficulties, the coordinator will contact the corresponding professionals according to his needs.
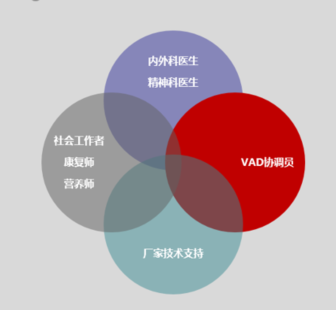
Schematic diagram of foreign VAD coordinator mechanism
Image source: provided by Liao Cui
In my country, a similar post-operative management system has yet to be established. At present, doctors and manufacturers are mainly assisted in the management of implanters.
Li Qianzhen said that in his hospital, within 1 year after the implant is discharged, he will come to the hospital for re-examination every three months. Years later, the frequency of re-examination was changed to once every six months.
Each patient implanted with a Cifu VAD meets 1 manufacturer’s engineer. During hospitalization, engineers will teach patients and families how to change batteries, maintain equipment, and review their operations. After being discharged from the hospital, they will return to the patient to clarify their doubts.
Liao Cui introduced that her engineers are on call 24 hours a day and can be contacted at any time. On the eighth day of the first month of this year, she made a mistake in taking a bath and the battery was soaked in water. Although the equipment did not alarm, the next day, the engineer who rushed from Suzhou to Wuhan accompanied her to Xiehe to replace the controller.
In the ward, Liao Cui’s postoperative doctor and a nurse connected her to ECG monitoring to observe her heart rate and blood pressure. Under the guidance of the engineer, the cable was pulled out of the old equipment, and Liao Cui’s pump stopped working temporarily. At that moment, she was extremely nervous.
After a few seconds, the pump was back on high speed as the cable was plugged into the new controller. Everything is back to normal.
Farewell to my pre-sick self
On September 14, 2021, on her 33rd birthday, Liao Cui received a gift from her husband: a lady’s leather bag, the color is her favorite light pink, which can be carried by hand or crossed diagonally , The straps are thin, which is also her favorite style.
After packing the battery and other equipment from the manufacturer’s package into a new bag, she found herself indistinguishable from the fashionable women on the street, not as conspicuous as before.

Liao Cui likes this full body photo
Image source: provided by Liao Cui
She is actively adjusting to her new life. She can no longer float and swim like she did before she got sick, so she develops new hobbies – reading books, putting on makeup, and playing table tennis and badminton with children in the same community. Unable to go out to work, she took care of the online fruit shop and worked hard to run the business better and better.
Liao Cui gradually fell in love with the current life: wake up at 7:30 every day, send Tiantian to kindergarten; work on time at 9:00; read a book or play a while in the afternoon, sleep for 1 hour Then take Tiantian home and take her to the square to play at 5 o’clock; after dinner, accompany Tiantian to read picture books, draw or practice calligraphy; when her daughter falls asleep, she goes back to work.
She was prepared to live with an artificial heart for the rest of her life. Before the doctor told her that the longest record of using an artificial heart abroad was 11 years, she made a wish in her heart: to create a new record.
Liu Yiming is also slowly saying goodbye to his pre-sick self. Last year, with the mentality of “if you can’t see it, you won’t miss it”, he gave all his badminton rackets, snowboards, and swimming equipment to others. Unexpectedly, after sending it out, he really let it go.
A deeper level of letting go occurs before the launch of the talk show. During that time, Liu Yiming kept asking himself: Can I go back to school and my previous life? Am I not accepting myself enough? In the end he gave the answer himself: it was time to start again.
In October 2021, Liu Yiming presents his first special performance “Fang Xinweiwei”. He hopes that he starts from his “heart” and looks at everything in the past from a different perspective, “You are reborn.”
Liu Cui had a similar idea. Before going to bed every night, the room became very quiet, and leaning on the pillow, she could clearly hear a “humming” sound. She knew it was the sound of the apex of the blood pump running round and round.
“What does it feel like to hear this sound?”
It means I’m alive, she said.
(Liu Yiming is a pseudonym in the text)
This article was reviewed by Li Qianzhen, Deputy Chief Physician of Cardiac Surgery, Union Hospital Affiliated to Fujian Medical University
Written by Su Zihan
Producer: Li Hualiang
Source of the first image: provided by Liao Cui
References:
1. Cardiovascular Branch of Chinese Medical Association, China Myocarditis Cardiomyopathy Collaborative Group. Guidelines for the diagnosis and treatment of dilated cardiomyopathy in China [J]. Journal of Clinical Cardiovascular Diseases, 2018, 34 (05):421-434.DOI:10.13201/j.issn.1001-1439.2018.05.001.
2. G Hao, X Wang, Z Chen, et al. Prevalence of heart failure and left ventricular dysfunction in China: The China Hypertension Survey, 2012-2015. Eur J Heart Fail 2019, 21: 1329-1337.
3. Wang Hua, Liang Yanchun. Chinese Heart Failure Diagnosis and Treatment Guidelines 2018 [J]. Chinese Journal of Cardiovascular Diseases, 2018, 46(10): 760-789.
Huang Jiefu. Report on the Development of Organ Transplantation in China (2019)[M]. Beijing: Tsinghua University Press, 2020.
4. Yu Xinyi, Liu Zhigang. Clinical application status and research progress of biventricular assist and total artificial heart [J]. Journal of Clinical Cardiovascular Diseases, 2021,37(10):964 -969.DOI:10.13201/j.issn.1001-1439.2021.10.018.
5. National Coverage Determination (NCD) 20.9.1 Ventricular Assist Devices (VADs)