Introduction:On September 20, ImmunoScape, a preclinical biotechnology company focused on the discovery and development of next-generation TCR-T cell therapies, announced that it has completed a $14 million deal. new round of financing. The round was led by existing investor Anzu Partner, with participation from new investor Amgen Ventures and Singapore-based global investor EDBI. Funds raised will be used to accelerate therapy development and advance candidate therapies into the clinic.
In recent years, in the field of solid tumor treatment, new immunotherapy represented by CAR-T therapy has achieved unprecedented breakthroughs. Among them, TCR-T therapy is also emerging. Due to its wider range of therapeutic targets, the potential of TCR-T in the treatment of solid tumors is worth looking forward to.
Cell receptor genetically engineered T-cell therapy (TCR-T therapy) is to transduce chimeric antigen receptors or TCRα/β heterodimers into ordinary T cells. Improve the affinity of T cell antigen receptors that specifically recognize tumor-related antigens and the fighting power of immune cells, thereby guiding T lymphocytes to exert a strong immune killing effect. TCR-T cell therapy has a bright future in the treatment of solid tumors. While CAR-T therapy is booming, related research on TCR-T therapy is also in full swing. Recently, ImmunoScape closed a $14 million financing to advance the discovery and characterization of cancer-specific T cell receptors.
Rare cancer-specific T cells discovered, ImmunoScape
$14 million in financing
ImmunoScape is a preclinical biotechnology company focused on the discovery and development of next-generation TCR-T cell therapies, and its Deep Immunomics platform leverages its proprietary There are combinatorial barcode technologies that enable the discovery and in-depth characterization of rare cancer-specific T cells and their T cell receptors at high resolution. It has extremely high sensitivity and can identify antigen-specific CD8-positive T cells with a frequency of only 0.001%[1]. This platform enables the simultaneous assessment of thousands of T cells in blood samples from hundreds of cancer patients to identify rare clinically relevant T cell clones, and then evaluate and prioritize corresponding TCRs to construct distinct TCR-T cells Therapeutic combination.

Regardless of sample type, the Deep Immunomics platform is able to mine T cells from peripheral blood and tumor-infiltrating lymphocytes. Its proprietary target screening platform, TargetScape, identifies hundreds of candidate T cells, routinely using the fetal-MHC encoding system with large antibody panels for high-throughput screening. These selected candidate T cells will be further subjected to single-cell sequencing to analyze their TCR sequence, phenotype, and gene expression. The identified TCR targets were further developed to analyze their efficacy, safety and efficacy through in vivo and in vitro models.
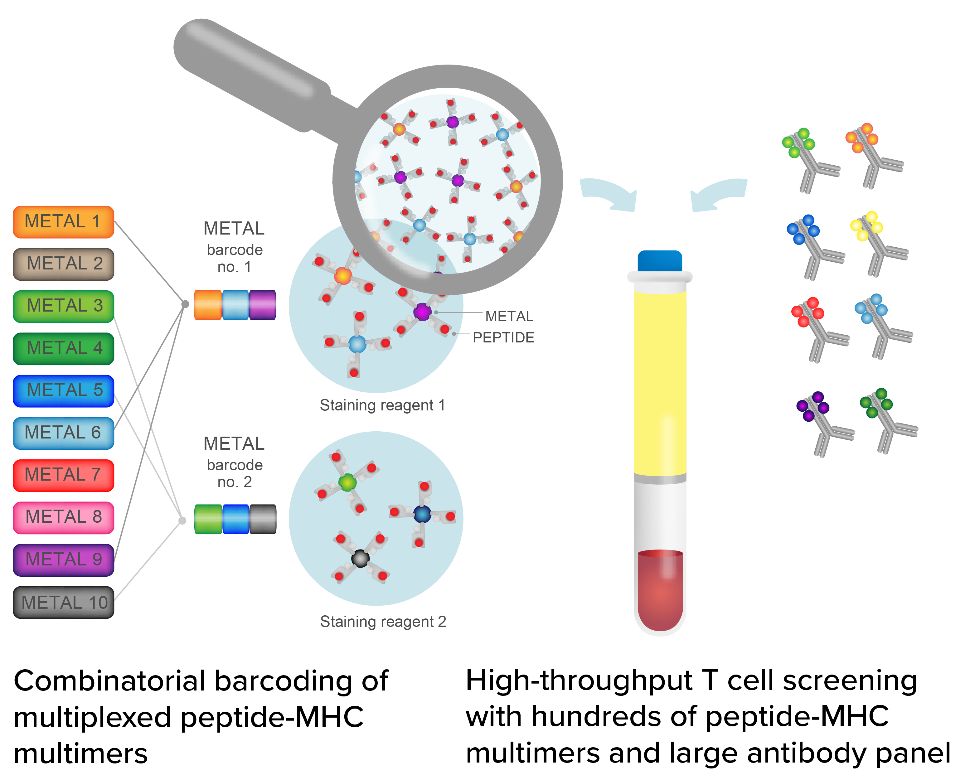
Figure 1 TargetScape, a target screening platform (Source: ImmunoScape official website)
That is, by utilizing computational biology and machine learning, as well as high-throughput screening and assessment of T cell clones, ImmunoScape is able to efficiently identify novel T cell therapeutic targets and TCR candidates The authors, who have extensively validated computational platforms using virus-specific T cells, are applying the same approach to build a broad portfolio of cancer-specific TCRs.
ImmunoScape CEO Choon Peng Ng said: “We have made significant progress in our discovery program and have identified several compelling clinical TCR candidates using our deep immunomics platform DeepImmunomics “The funds raised will allow us to accelerate our development efforts and help advance therapeutic candidates into the clinic. We are delighted to have the support of Amgen Ventures and look forward to working with their team to leverage ImmunoScape’s technology to address important and unmet medical needs.” .”
Amgen Ventures Vice President Philip Tagari said, “Amgen Ventures is committed to investing in promising solutions to address healthcare’s greatest challenges, especially those that offer a unique, value-based approach. Solutions, these approaches are consistent with our mission to serve patients. As we continue to develop the next generation of innovative medicines, ImmunoScape’s deep immunomics and machine learning platform has the potential to help discover new therapeutic options. It is a pleasure to work with the team at ImmunoScape Collaborate to unleash the full power of its technology.”
The TCR-T of the “tumor buster” is emerging in the treatment of solid tumors
In 2006, Morgan et al. first reported the use of MART-1-specific TCR-T cells in the treatment of melanoma with an objective response rate of 12%, proving that TCR-T lymphocytes Feasibility of treatment in clinical application. In 2011, Robbins et al. first demonstrated the clinical efficacy of NY-ESO-1-specific TCR-T cells in patients with melanoma and synovial sarcoma. The objective response rate in the tumor group was 55%[2].
In 2014, the Rosenberg team treated a late-stage patient with a point mutation in ERBB2IPFor patients with refractory cholangiocarcinoma, after receiving the infusion of neoantigen-reactive immune cells, the survival time of the patients was significantly prolonged, and the disease was continuously relieved, which caused a sensation in the academic circles. Since then, the target of TCR-T cell therapy has been extended to individualized neoantigens. Multi-target reactive T cells can simultaneously recognize multiple antigens by integrating multiple antigen information, and to a certain extent improve the resistance of T cells. Tumor effect.
Neither on-target autoimmune toxicity nor off-target cross-reactivity occurs in healthy tissue. Neoantigen TCR-T cells have been used to treat solid tumors, such as melanoma, metastatic colorectal cancer, glioblastoma, metastatic HPV16-positive cervical cancer, anal cancer, oropharyngeal cancer, and vaginal cancer, with satisfactory results. The above shows that TCR-T has shown great therapeutic potential and advantages in the field of solid tumor therapy.
Solid tumor killer TCR-T, how far is it from clinical application?
Compared with CAR-T, TCR-T can better infiltrate solid tumors and is highly sensitive to antigens, indicating that TCR-T has more significant advantages in the field of solid tumor treatment . Although TCR-T has shown great therapeutic potential in preclinical and clinical studies, there are still many unavoidable challenges.
■ Lack of suitable neoantigen targets
Choosing new and safe targets is the biggest challenge in tumor immunotherapy. First, low neoantigen load and MHC downregulation make tumor cells lose neoantigen targets. In cancers with a low mutational burden, few or no neoantigens are present, making subsequent studies of neoantigen-specific TCR-T impossible. Some tumors have immune evasion phenomena such as HLA downregulation and neoantigen loss, resulting in a lack of T cell recognition targets on the tumor cell surface. Second, lack of universal neoantigen targets. The clinical application of neoantigen-specific T cell therapy technology is limited to case reports and does not have universal application value. Due to the lack of universal neoantigen targets, the cost of neoantigen-targeted TCR-T cell therapy presents a new challenge for every patient. Third, HLA restrictions will limit the application of TCR-T. Current TCR therapies rely on matching HLA, but many patients have limitations in HLA typing.
■Off-target and safety issues in TCR gene transfer
Since engineered TCR-T cells cannot differentiate between tumor cells and normal cells expressing the target antigen, TCR-T cell immunization may severely damage the corresponding normal tissues. Off-target events during TCR therapy treatment may be caused by self/cross-reactivity between heterodimers containing two alpha chains and two beta chains, which may lead to new autoimmune specificities. TCR dimer-dependent mixed toxicity may also become a safety issue in clinical applications [3].
■Tumor antigen heterogeneity and tumor immune escape
The expression of cancer-associated antigens varies among different cells within a tumor, allowing some tumor cells to evade specific antigen-targeted therapy and leading to some receiving immune checkpoint inhibitors and Treatment resistance develops in patients treated with adoptive T cells. Tumor immune escape refers to the ability of tumor cells to survive and proliferate in the body by avoiding recognition and attack by the immune system through various mechanisms. Solid tumors are characterized by a complex immunosuppressive microenvironment and inherent heterogeneity, making durable TCR-T-induced responses difficult[3].
In addition to the above three problems, TCR-T also faces challenges such as T cell anergy and exhaustion, and toxicity caused by cytokine storm.
In summary, TCR-T still has significant advantages in the treatment of solid tumors, but there are still many inevitable problems. It is believed that with the development of various technologies, these challenges will be solved one by one, and TCR-T cell therapy will definitely become an “anti-cancer weapon”.
Writing | Mu Zijiu
Typesetting|Text Competition
References:
[1]https:https://immunoscape.com/immunoscape-raises-14m-to-facilitate-the-discovery-and-characterization-of-cancer-specific-t-cell -receptors/
[2]Xu R, Du S, Zhu J, et al. Neoantigen-targeted TCR-T cell therapy for solid tumors: How far from clinical application. Cancer Lett. 2022 Oct 10; 546:215840. doi: 10.1016/j.canlet.2022.215840. Epub 2022 Jul 31. PMID: 35921969.
[3]Liu Y, Yan X, Zhang F, et al. TCR-T Immunotherapy: The Challenges and Solutions. Front Oncol. 2022 Jan 25;11:794183. doi: 10.3389/ fonc.2021.794183. PMID: 35145905; PMCID: PMC8822241.
This article is an original creation of biological exploration. Personal forwarding and sharing are welcome. If any other media or website needs to be reprinted, the source Biological Discovery must be indicated before the text.